Many practices report that provider credentialing now takes 90-180 days or more before reimbursement begins, compared to much shorter timelines in previous years. Practices that do not complete credentialing on time frequently lose thousands of dollars in billable revenue each month per provider, with slow CAQH credentialing remaining a significant contributor to these delays.
The CAQH Provider Data Portal is one of the primary centers where payers validate provider credentials. The database contains more than 4.8 million provider records, and over 1,000 health insurers use CAQH data for credentialing and directory administration. This centralization reduces duplicated work and increases data accuracy, only if the profiles are complete and up to date.
Most credentialing delays are caused by insufficient or outdated CAQH information, missed re-attestation cycles, and inconsistencies between payer systems and credentialing platforms. Delays in CAQH credentialing directly result in delayed enrollment, reimbursement holds, and operational setbacks for physicians, billing teams, and revenue cycle specialists.
What Is CAQH Credentialing and Why Does It Matter?
CAQH credentialing is the process of creating and maintaining a centralized provider profile in the CAQH Provider Data Portal. Health plans use this profile to verify professional data and make network participation decisions. Accurate data here is essential for enrollment, claims processing, and directory compliance.
Providers and credentialing teams must understand the role CAQH plays in payer decisions. Any error or outdated information can delay payer approval. Delays here extend credentialing timelines and slow revenue cycles. Errors also increase administrative follow‑up and workload for billing staff and credentialing specialists.
Updated CAQH profiles reduce repeated requests for documents from payers. This enables credentialing teams to focus on pending applications instead of correcting repetitive data. For revenue cycle professionals, accurate CAQH data supports faster claim acceptance.
Role of CAQH in Provider Enrollment
CAQH centralizes provider data for multiple health plans. Key functions include:
- Collecting licensure, DEA, and board certifications
- Documenting work history, education, and practice addresses
- Tracking disclosures like sanctions or malpractice claims
- Allowing payers to verify credentials without repeated submissions
Who Uses CAQH Credentialing Data
CAQH data is critical for:
- Commercial health plans: Confirm provider qualifications before network acceptance
- Credentialing specialists and administrators: Streamline enrollment for groups and solo practices
- Revenue cycle and billing teams: Validate provider status to avoid claim rejections
- Healthcare providers: Maintain accurate information for faster reimbursement
CAQH Credentialing Process Explained
This section explains how providers submit, verify, and maintain credentialing data through CAQH. It focuses on accuracy, compliance, and avoiding delays that affect enrollment and reimbursement.
CAQH credentialing uses a single provider profile to support enrollment with multiple commercial payers. The process requires structured data entry, document uploads, payer authorization, and periodic confirmation. Errors at any point can cause enrollment to be paused or delayed.
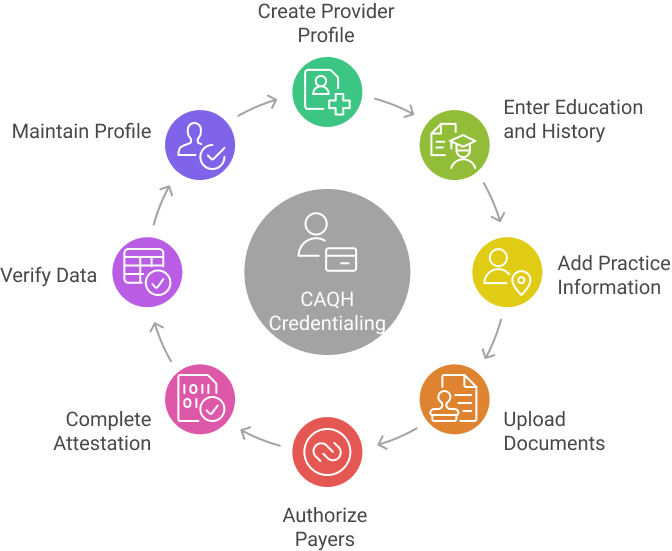
Creating a CAQH Profile for Providers
Providers’ CAQH profiles serve as the foundation for payer enrollment. Most commercial insurers check this profile before allowing a network.
Key steps include:
- Register using NPI, SSN, license number, and contact details.
- Enter education, training, and work history with gap explanations
- Add practice locations, tax ID, and billing contacts
- Upload licenses, DEA certificate, malpractice insurance, and CV
- Authorize payers to access the profile
- Complete electronic attestation
CAQH Application for Doctors and Non-Physician Providers
The CAQH application for doctors and non-physician providers follows the same structure but varies by provider type.
Physicians typically submit:
- Board certifications
- Hospital affiliations
- Admitting privileges, when required
Non-physician providers may need:
- Supervising physician details
- Scope-of-practice documentation
- State-specific approvals
How to Complete the CAQH Profile Correctly
This section explains how providers should complete and maintain their CAQH profile to avoid delays. It focuses on required data standards and the most frequent errors that impact payer review.
Completing the CAQH profile correctly is a core requirement for CAQH credentialing. Health plans rely on this data to confirm provider eligibility, verify credentials, and approve enrollment. Inaccurate or incomplete profiles are a leading cause of stalled applications.
Required Documents and Data Standards
A CAQH profile for providers must meet uniform data standards used by commercial payers. All fields marked as required must be complete before payers can access the profile.
Providers must upload and maintain:
- Active state licenses for each practice location
- DEA registration, if applicable
- Malpractice insurance with current limits and dates
- Board certifications or specialty credentials
- Education, residency, and fellowship records
- Complete work history with gap explanations
- Practice addresses, tax ID, and billing contacts
- Hospital affiliations, when required
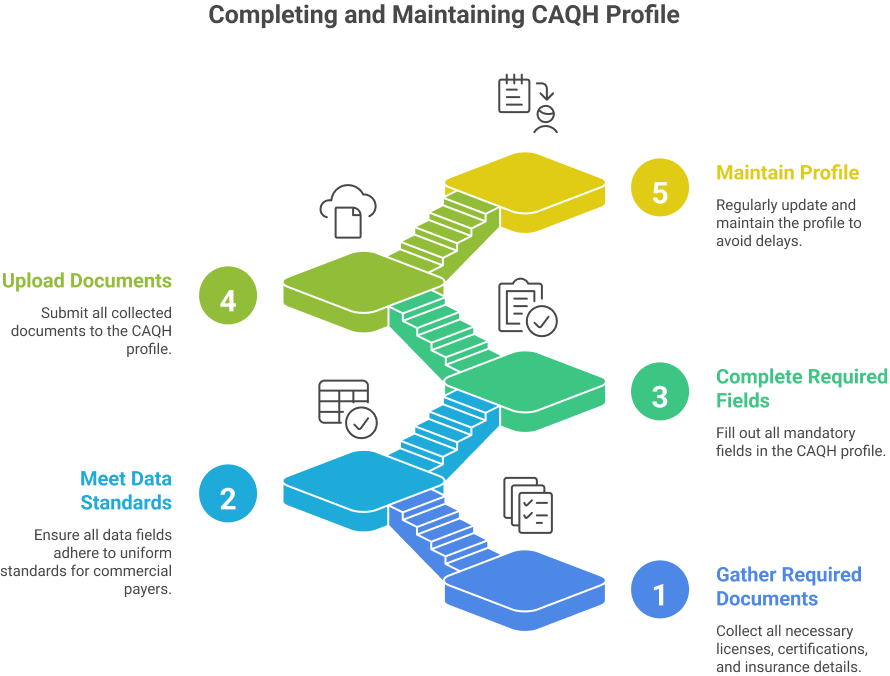
Common Data Entry Errors
Common CAQH credentialing errors delay enrollment and increase follow-up requests.
Frequent issues include:
- Missed CAQH re-attestation requirements every 120 days
- Name or address differences between CAQH and NPPES
- Missing work history dates or unexplained gaps
- Uploading expired malpractice or license documents
- Failing to authorize payer access
- Incorrect provider type selection
CAQH Re-Attestation Requirements
This section describes how re-attestation works, when scheduling is important, and how missed deadlines impact enrollment. It focuses on preventing profile inactivity and payment delays related to CAQH credentials.
Re-attestation confirms that provider data stored with Council for Affordable Quality Healthcare remains current and accurate. Payers rely on this confirmation before continuing credentialing reviews or appealing claims.
Re-Attestation Schedule and Notifications
CAQH re-attestation requirements apply every 120 days. All providers must review their profile, update changes, and submit an electronic confirmation.
Key points include:
- Re-attestation is mandatory, even if no data changes
- Email reminders are sent before the due date
- Profiles remain active only after confirmation is submitted.
- Group administrators can track the status of affiliated providers
What Happens When Re-Attestation Is Missed
A missed re-attestation renders the profile inactive. Providers cannot access inactive profiles.
Common consequences include:
- Credentialing applications are placed on hold
- Delayed network approvals
- Claim denials due to inactive provider records
- Additional document requests from payers
- Extended enrollment timelines
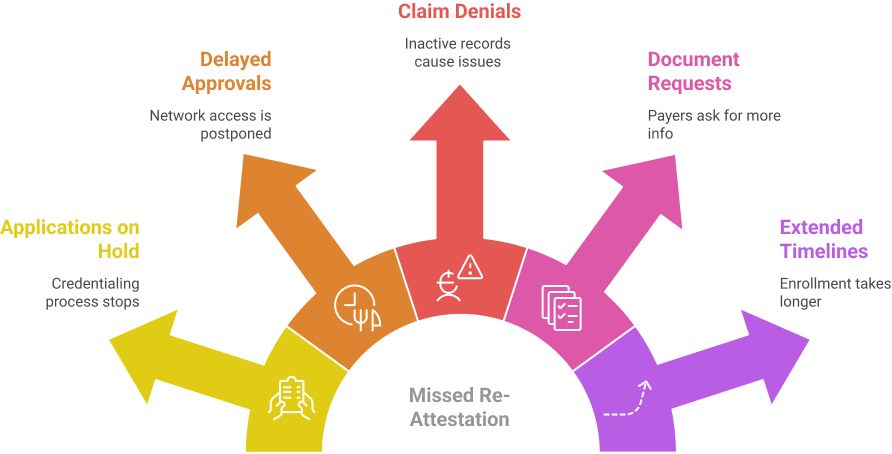
Common CAQH Credentialing Errors That Delay Enrollment
This section explains common CAQH credentialing issues that stall approvals and interrupt billing. It focuses on errors that have a direct impact on enrollment timeframes and reimbursements.
Many delays occur due to preventable data issues inside the Council for Affordable Quality Healthcare system. Payers often pause applications until these errors are corrected.
Errors Linked to Revenue Cycle Disruption
The following issues appear most often during payer review and directly impact cash flow:
Expired documents
Licenses, DEA certifications, or malpractice policies expire and prevent verification.
Missed re-attestation
Failure to confirm data every 120 days causes profile inactivation.
Data mismatches
Differences between CAQH, NPI, PECOS, or payer files trigger manual reviews.
Incomplete work history
Gaps without explanations raise compliance concerns.
Incorrect practice details
Wrong tax ID, address, or billing contact delays contract setup.
Payer access not granted
Profiles remain invisible when authorization is missing.
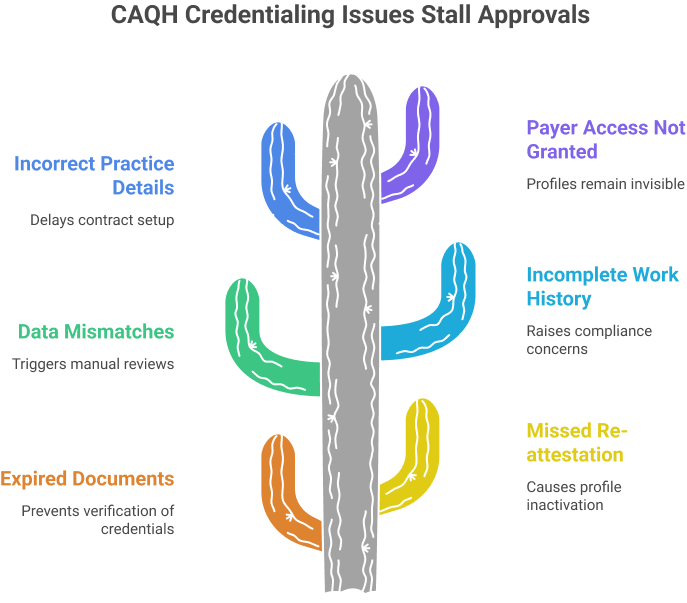
How Enrollment Teams Can Prevent These Errors
Enrollment teams can reduce delays by applying consistent controls:
- Audit CAQH profiles monthly for expirations
- Align CAQH data with NPPES and PECOS records
- Track re-attestation dates using shared calendars
- Confirm payer access before submitting applications
- Validate work history entries during onboarding
CAQH Credentialing Best Practices for Long-Term Compliance
This section explains how teams should keep accurate provider data across time and minimize enrollment disruptions. It focuses on measures that promote stable payer access via CAQH credentialing.
Long-term compliance depends on consistent data checks and shared accountability across departments using the Council for Affordable Quality Healthcare platform.
Internal Controls for Credentialing Teams
Credentialing teams require specific controls to maintain a current and payer-ready list.
Effective practices include:
- Assigning a single owner for each CAQH profile
- Tracking license, DEA, and insurance expiration dates monthly.
- Reviewing work history for gaps before payer submission
- Verifying practice locations, tax IDs, and billing contacts quarterly
- Maintaining an internal log of payer access approvals
- Confirming re-attestation completion every 120 days
- Use a checklist before each payer submission
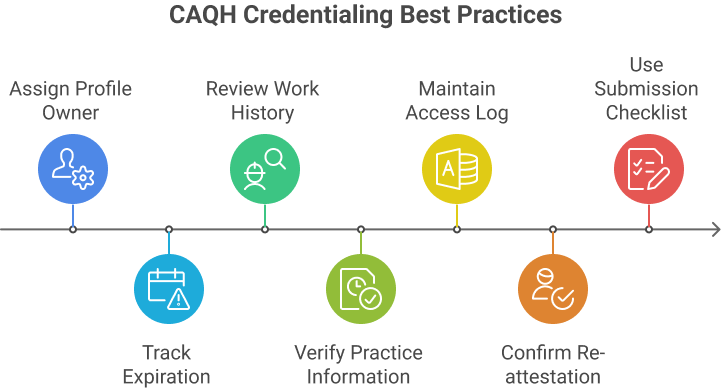
Alignment Between Credentialing and Billing Teams
Credentialing and billing teams must share the same provider data. Misalignment causes enrollment delays and claim holds.
Coordination steps include:
- Matching CAQH data with NPI and PECOS records
- Sharing payer approval dates before claims are filed
- Confirming billing addresses and rendering details before go-live
- Flagging enrollment gaps that affect reimbursement
Holding joint reviews during onboarding and role changes
Conclusion
CAQH credentialing has a direct impact on enrollment speed, payer approval, and reimbursement timelines. Incomplete data, missed re-attestation, or system mismatches continue to delay revenue for providers and billing teams.
Accurate profiles, routine controls, and coordination between credentialing and billing teams reduce enrollment holds. Consistent oversight of CAQH data supports stable network participation and predictable cash flow.
FAQs
What is CAQH credentialing, and why is it required?
CAQH credentialing enables payers to validate provider data using a single centralized profile. Incomplete data frequently causes delays in registration and reimbursement.
How long does CAQH credentialing take for providers?
CAQH profile completion can take days, and payer review typically extends the entire credentialing process to 90-180 days if concerns arise.
How often must providers complete CAQH re-attestation?
Providers must re-attest their CAQH profile every 120 days. Missing this deadline causes profile inactivity and enrollment delays.
What are the most common CAQH credentialing errors?
Expired documents, data mismatches, missing work history, and failure to grant payer access are the most frequent causes of delays.
Who should manage the CAQH profile in a practice?
Credentialing or enrollment teams should own CAQH profile management, with coordination from billing teams to avoid claim holds.





