Are you prepared for how Medicare and Medicaid credentialing may impact your practice in 2026? Providing services to people enrolled in these programs is an essential source of revenue for many healthcare providers. In 2025, around 68.9 million Americans were registered in Medicare, with the majority being 65 or older. As the population ages, the demand for provider participation will increase. Approximately 76.8 million people were covered by Medicaid and CHIP, with 69.5 million enrolled worldwide.
In order to assist such individuals and get reimbursement, providers must satisfy the necessary certification and enrollment requirements. Credentialing and enrolling are independent processes. Credentialing confirms your qualifications, training, and licensure. Enrollment provides the ability to bill federal and state programs. Skipping or misunderstanding either stage can prevent reimbursements and limit access to covered patients.
This article outlines the steps required for Medicare provider enrollment through PECOS, discusses how Medicaid enrollment varies by state, and emphasizes typical errors that result in delayed or denied claims. Accurate credentialing and enrollment have a direct impact on a practice’s capacity to bill federal and state payers in 2026 and later.
Medicare and Medicaid credentialing
This section explains the difference between credentialing and enrollment. It also discusses why many providers delay claims or face denials. The goal is to position credentialing and enrollment as separate but connected stages that directly affect billing and reimbursement.
Credentialing vs Enrollment: What Providers Often Miss
Credentialing verifies a provider’s education, training, license status, board certifications, and sanctions history. It confirms qualifications to serve patients. Medicare and Medicaid credentialing begin with these verifications. Providers must show compliance with federal and state requirements. Primary source verification is required for Medicare provider enrollment and for most state Medicaid enrollment systems.
Enrollment authorizes a provider to bill a payer for services. Under Medicare, enrollment occurs through PECOS enrollment with the Centers for Medicare & Medicaid Services. For Medicaid, enrollment happens through state Medicaid agencies. Enrollment follows credentialing evidence. Approval establishes an effective date for billing.
Many providers assume credentialing equals enrollment. This assumption leads to denied claims, delayed reimbursements, and audit risk. Credentialing alone does not grant billing privileges. Claims submitted before enrollment approval are non‑payable. Providers must check the effective dates issued by PECOS or state systems before billing.
Medicaid provider credentialing varies by state. Each state sets its own screening levels and documentation rules. Some states require fingerprint checks, site visits, or managed care organization (MCO) enrollments separate from fee‑for‑service. Providers who ignore these state procedures face extended delays and limited patient reach.
Credentialing teams and medical billing specialists must ensure that credentialing data matches enrollment applications. Discrepancies between education, licensure, and practice location are common errors. These errors cause rejection of PECOS enrollment or state Medicaid enrollment and postpone claim acceptance.
Understanding the difference between credentialing and enrollment protects revenue cycle teams from preventable denials. It also ensures compliance with federal and state billing standards.
Medicare Provider Enrollment Process
This section covers the Medicare provider enrollment steps and common pitfalls. Understanding these steps ensures timely approval and prevents claim delays for credentialed providers.
Medicare Provider Enrollment Steps
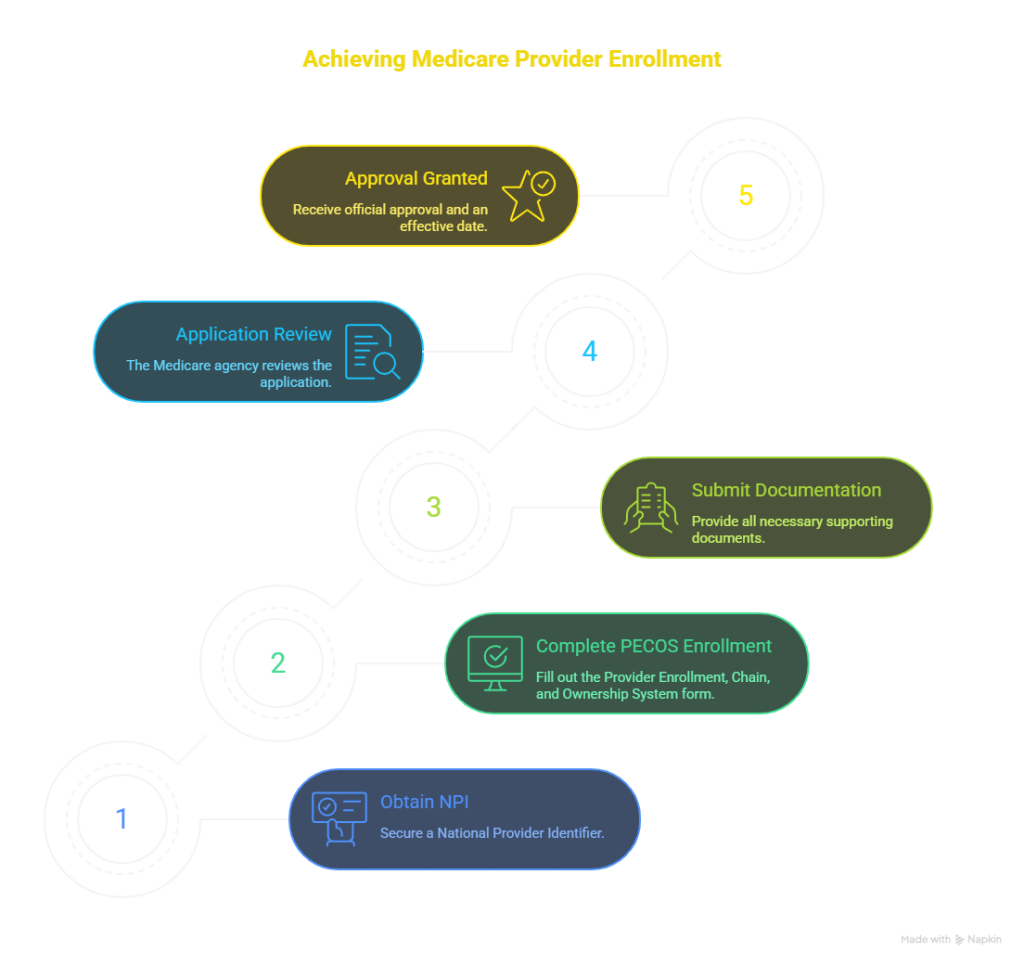
Medicare provider enrollment is the process that allows qualified providers to bill Medicare for services. It starts after credentialing verification. The steps include:
1. Obtain an NPI: Providers must have an active National Provider Identifier (NPI) before enrolling.
2. Complete PECOS Enrollment: Use the PECOS enrollment system for online submission. Include all practice locations, licenses, and liability coverage details.
3. Submit Required Documentation: Attach medical licenses, board certifications, DEA registrations, and malpractice coverage.
4. Application Review: CMS or Medicare Administrative Contractors (MACs) review all submissions. Verify primary sources and check for sanctions.
5. Approval and Effective Date: Upon approval, Medicare issues an effective enrollment date. Only after this date can providers bill Medicare.
PECOS Enrollment Errors That Delay Claims
Many providers face delays due to errors in PECOS submissions. Common mistakes include:
- Mismatched provider name, license, or NPI information.
- Missing or expired licenses and DEA certificates.
- Incorrect or incomplete practice location details.
- Failure to disclose adverse legal or sanction history.
- Not confirming effective dates before billing.
Medicaid Provider Credentialing by State
Medicaid provider credentialing requirements vary by state. Understanding these differences ensures providers complete enrollment accurately and avoid claim denials or payment delays.
State Medicaid Enrollment Differences
Each state manages state Medicaid enrollment independently. Key differences include:
- Application Systems: Some states use online portals, others require paper forms.
- Documentation Requirements: License verification, DEA registration, malpractice coverage, and board certification may differ by state.
- Processing Times: Enrollment can take 2–12 weeks, depending on the state and completeness of documentation.
- Provider Types: Certain states require separate enrollment for hospitals, clinics, or DMEPOS suppliers.
Common State-Level Medicaid Delays
Providers often encounter delays due to errors or missing documentation. Common issues include:
- Incomplete or inconsistent provider information.
- Failure to submit required supporting documents, such as a license or malpractice coverage.
- Delays in state verification of credentials or sanctions.
- Not updating practice locations or ownership changes promptly.
- Misalignment between Medicaid and PECOS records for dual Medicare/Medicaid providers.
Provider Enrollment Services vs Internal Enrollment
Choosing between using external provider enrollment services or handling enrollment internally can impact timelines, compliance, and revenue. Understanding the differences helps practices reduce errors and expedite credentialing.
When Internal Teams Are at Risk
Internal enrollment teams often face challenges that can delay Medicare and Medicaid credentialing:
Limited Staff Expertise: Internal teams may lack up-to-date knowledge of PECOS enrollment, state Medicaid enrollment, or insurance-specific requirements.
High Workload: Managing credentialing alongside other administrative duties increases the risk of errors.
Documentation Gaps: Missing license verification, DEA registration, or malpractice information can lead to application rejection.
Compliance Oversight: Staying current with federal and state updates is difficult, exposing providers to audit risk.
Delayed Revalidation: Without dedicated staff, re-enrollment and re-credentialing deadlines can be missed, causing lapses in billing privileges.
Common Mistakes Providers Make in Medicare and Medicaid Credentialing
Even experienced practices encounter errors that delay approvals, disrupt billing, and increase compliance risk. Understanding these common mistakes helps prevent denials and lost revenue.
Incomplete or Inaccurate Applications
Many delays stem from missing documents or mismatched information:
- Incorrect or expired licenses
- Missing DEA registration or state-controlled substance certificates
- Inaccurate practice addresses or Tax ID numbers
- Gaps in work history or training verification
Overlooking Revalidation and Renewal Deadlines
Failure to monitor re-enrollment schedules for Medicare and state Medicaid programs is frequent:
- Missing PECOS revalidation dates can suspend billing privileges.
- State Medicaid enrollment deadlines vary, and lapses prevent claim submissions.
- Ignoring annual insurance provider updates can result in denied claims
Ignoring State-Specific Requirements
Each state enforces unique Medicaid provider credentialing rules:
- Some states require additional criminal background or fingerprint checks
- Documentation for multi-state providers must meet every state’s regulations.
- Delays occur when providers assume federal rules override state-specific steps
Relying Solely on Internal Teams
Internal teams without specialized expertise often miss critical steps:
- Misunderstanding PECOS enrollment workflows
- Submitting incomplete provider enrollment applications
- Failing to track credentialing status across multiple insurers
Conclusion
Accurate Medicare and Medicaid credentialing is essential for uninterrupted billing and compliance in 2026. Providers who verify credentials, complete PECOS and state Medicaid enrollment correctly, and monitor revalidation deadlines reduce claim denials and protect revenue.
Relying on internal teams alone or overlooking state-specific requirements increases delays and audit risk. Combining expert provider enrollment services with structured internal oversight ensures timely approvals, full reimbursement, and consistent patient access across federal and state programs.
FAQs
What is the difference between Medicare and Medicaid credentialing and enrollment?
Credentialing verifies provider qualifications and compliance. Enrollment grants billing rights with Medicare or state Medicaid programs.
How long does Medicare provider enrollment take through PECOS?
In 2026, PECOS enrollment typically takes 30–90 days, depending on application accuracy and MAC review timelines.
Why does Medicaid provider credentialing differ by state?
Each state Medicaid agency sets its own screening level, documentation rules, and approval timelines under federal guidance.
Can providers bill before Medicare or Medicaid enrollment approval?
No. Claims submitted before the approved effective date are non-payable and will be denied without appeal rights.
What are the most common mistakes that delay credentialing and enrollment?
Incomplete applications, data mismatches, missed revalidation deadlines, and ignoring state-specific Medicaid requirements.





