The hospital’s privileging process has an impact on patient care, revenue, and compliance. Many hospitals continue to rely on manual workflows, which slow approvals. More than half of healthcare organizations anticipate revenue losses due to credentialing and privileging delays by 2026, with some losing more than $1 million per year because providers cannot bill until approvals are completed. These delays also increase the time it takes for a new practitioner to see patients.
Providers and revenue teams face friction at several stages. On average, credentialing and privileging workflows take 90-120 days from application to final approval, causing a time when providers cannot generate billable encounters. Extended onboarding leads to increased claim denials, cash flow delays, and administrative load across departments.
Understanding hospital privileging requirements, distinctions from credentialing and enrollment, and common bottlenecks is essential for physicians. This blog breaks down the hospital privileging process, highlights requirements, explains how it works, and shows how these procedures affect billing, compliance, and operational performance in today’s healthcare environment.
What Is the Hospital Privileging Process
The hospital privileging process defines the scope of care a provider can deliver within a facility. Proper privileging ensures qualified providers perform appropriate procedures safely and legally.
Purpose of Hospital Privileging
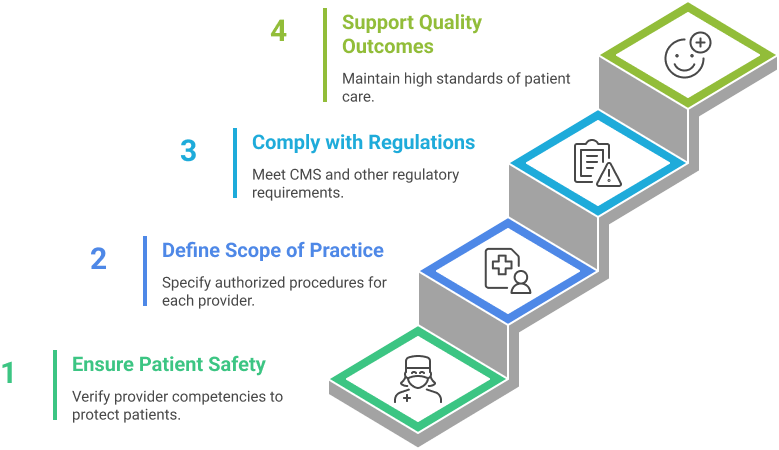
Hospital privileges determine which clinical procedures and services each provider can perform. Its purposes include:
- Ensuring patient safety: Only providers with verified competencies deliver care.
- Defining scope of practice: Privileges specify procedures a provider is authorized to perform.
- Compliance with regulations: CMS and other regulatory bodies require documentation of privileges.
- Supporting quality outcomes: Privileged providers meet facility standards and maintain consistent patient care.
Who Oversees Privileging Decisions
Oversight of privileging is shared between the Medical Staff and the Governing Body:
- Medical Staff: Reviews individual provider applications, verifies credentials, assesses clinical competence, and recommends privileges. Reviews typically include education, training, board certifications, malpractice history, and peer evaluations.
- Governing Body: Grants final privileges, ensures compliance with hospital policies and regulatory requirements, and informs departments of the privileges granted. Only the governing body can approve, limit, or revoke privileges.
Hospital Privileging Requirements
Hospitals must consider each provider independently before giving privileges. Compliance with the CMS Conditions of Participation (CoPs) and state requirements is required. In 2026, almost 48% of hospitals reported delays in privileging due to insufficient documentation or a lack of validated competencies, emphasizing the importance of clear rules and thorough examination.
Core Privileging Criteria
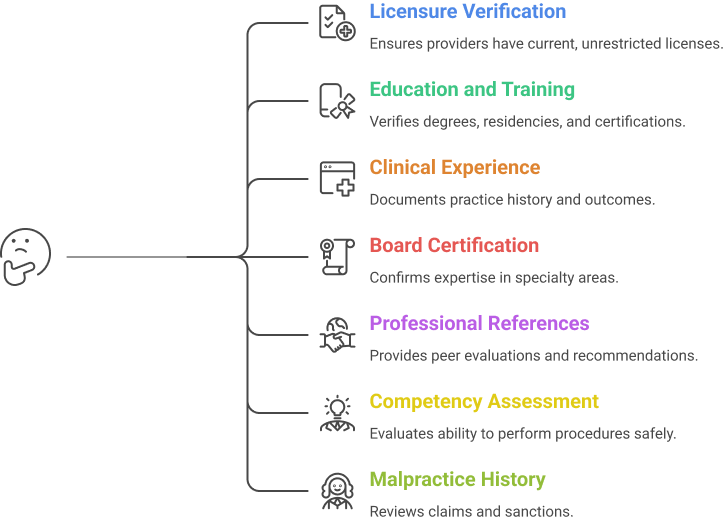
Hospitals assess providers using standardized criteria to ensure patient safety and operational compliance. Core privileging requirements typically include:
- Licensure Verification: Current, unrestricted medical or professional license.
- Education and Training: Verified degrees, residencies, fellowships, and relevant certifications.
- Clinical Experience: Documented practice history, procedure logs, and outcomes.
- Board Certification: When applicable, in the provider’s specialty area.
- Professional References: Peer evaluations and recommendations from supervisors or collaborators.
- Competency Assessment: Ability to perform requested procedures safely within hospital resources.
- Malpractice and Disciplinary History: Review of claims, sanctions, and NPDB reports
How Hospital Privileging Works
The hospital privileging process defines how healthcare providers are authorized to perform specific clinical services. This ensures care is delivered safely and within the provider’s competencies.
Step-by-Step Privileging Workflow
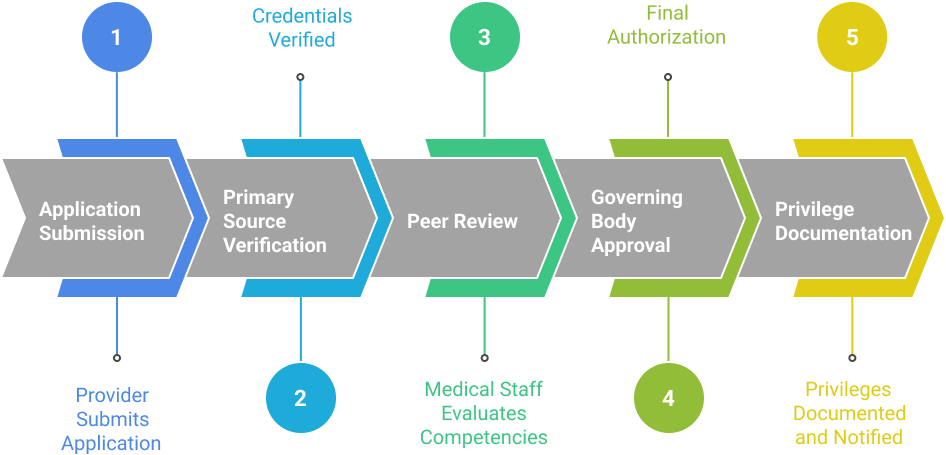
Hospitals follow a standardized workflow to grant privileges efficiently while maintaining compliance:
1. Application Submission: Providers submit detailed applications, including licenses, training records, clinical experience, board certifications, and references.
2. Primary Source Verification: Verification of credentials, employment history, malpractice claims, and regulatory compliance through NPDB, OIG/SAM checks, and state licensing boards.
3. Peer Review: Medical staff evaluates the provider’s competencies against hospital-defined criteria and recommends privileges.
4. Governing Body Approval: Final authorization of privileges rests with the hospital governing body.
5. Privilege Documentation: Hospitals document approved privileges, limitations, or restrictions and notify relevant departments and staff.
Ongoing Monitoring
Privileges are not static. Hospitals must continuously review provider performance and competencies to maintain patient safety:
- Periodic Re-evaluation: Privileges must be reviewed at least every 24 months or sooner if required by state law.
- Performance Audits: Clinical outcomes, procedure logs, peer feedback, and adverse events are evaluated.
- Privilege Modification or Revocation: Any limitation or revocation must be documented and reported to NPDB and relevant authorities.
- Continuous Compliance: Hospitals track credentialing expiration, continuing education, and regulatory updates to ensure ongoing compliance.
Credentialing vs Privileging
Credentialing and privileging are related but distinct processes in hospital administration. Understanding the difference ensures providers meet compliance standards and deliver safe care.
Differences Between Credentialing and Privileging
Here is the difference between credentialed and privileged.
| Process | Definition | Purpose | Outcome |
| Outcome | Verification of qualifications, licenses, education, training, and professional history | Authorization to perform specific procedures or services within the facility | Provider is authorized to work in the hospital or network |
| Privileging | Authorization to perform specific procedures or services within the facility | Provider is authorized to work in the hospital or network | Define the scope of practice based on competencies |
Physician Privileging Checklist
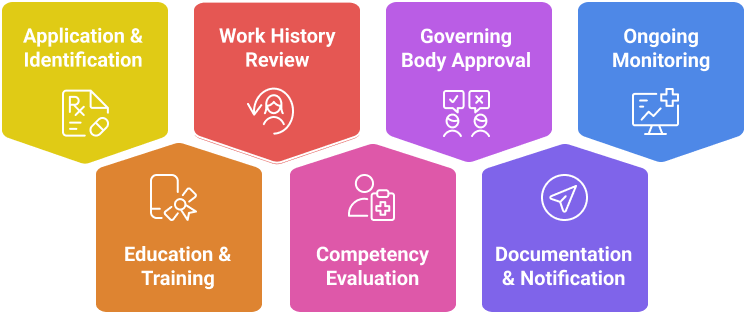
A standardized checklist ensures no step is missed when granting privileges:
1. Application and Identification: Include medical license, DEA registration, board certification, and malpractice history.
2. Education and Training Verification: Confirm medical school, residency, fellowship, and continuing education records.
3. Work History Review: Assess prior employment, hospital affiliations, and relevant clinical experience.
4. Competency Evaluation: Peer review of clinical skills, surgical procedures, and outcomes data.
5. Governing Body Approval: Hospital leadership validates the recommended privileges.
6. Documentation and Notification: Communicate approved privileges to all relevant departments.
7. Ongoing Monitoring: Conduct periodic re-privileging and performance evaluation every 24 months or as state law requires.
Types of Hospital Privileges
Hospital privileges determine what procedures a provider can perform safely within a facility. Understanding these types ensures the proper scope of practice and compliance with medical staff standards.
Common Privilege Categories
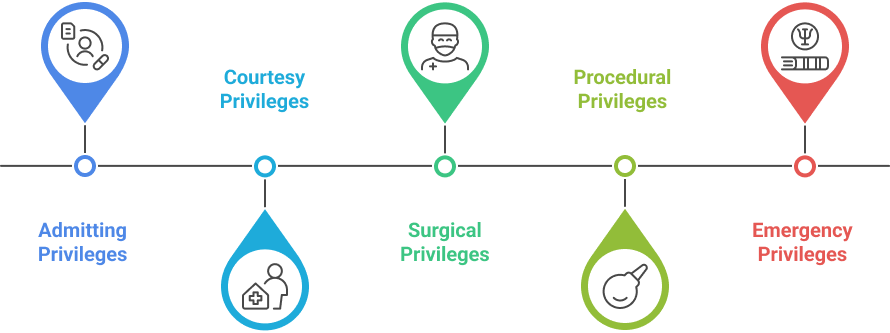
Hospital privileges are generally divided into broad categories to match clinical responsibilities:
1. Admitting Privileges
- Allow physicians to admit patients for treatment.
- Commonly granted to primary care providers, specialists, and surgeons.
2. Courtesy Privileges
- Allow providers to treat or consult on patients without full membership on the medical staff.
- Often used for visiting physicians or part-time providers.
3. Surgical Privileges
- Authorize performance of procedures in operating rooms or specialized units.
- Limited to providers with verified surgical training and competency records.
4. Procedural Privileges
- Cover non-surgical interventions like endoscopy, imaging-guided procedures, or anesthesia administration.
- Granted after peer review and skills assessment.
5. Emergency Privileges
- Temporary privileges for urgent situations or newly arriving practitioners.
- Must comply with hospital and CMS standards for emergency care.
Specialty-Specific Limitations
Privilege scope is often restricted by specialty and hospital capability:
Cardiology: Procedures limited to catheterization labs or interventional suites based on training.
Anesthesiology: Privileges may vary for CRNAs versus anesthesiologists, depending on supervision rules.
Obstetrics/Gynecology: Delivery privileges granted after verified experience with cesarean sections or high-risk cases.
Orthopedics: Surgical privileges restricted to joint replacements or fracture management, depending on board certification.
Radiology: Limited to imaging modalities and procedures supported by hospital equipment and staff.
Physician Privileging Checklist
A physician’s privileging checklist ensures hospitals verify qualifications, experience, and competence before granting privileges. This safeguards patient safety and maintains compliance with regulatory standards.
Required Documentation
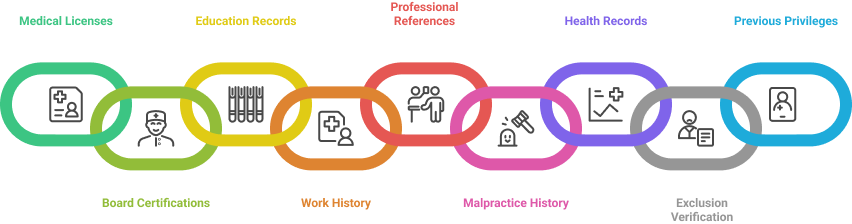
Hospitals require detailed documentation to support privileging decisions. Core items include:
Medical Licenses: Current state licenses and federal DEA registration.
Board Certifications: Proof of board certification or recertification in the relevant specialty.
Education and Training Records: Medical school diploma, residency, fellowship certificates, and continuing education history.
Work History: Complete employment and practice affiliations, including privileges at other facilities.
Professional References: Peer evaluations and recommendations from previous supervisors or colleagues.
Malpractice and Claims History: Detailed history of past claims and resolution outcomes.
Immunization and Health Records: Evidence of immunizations and TB screening, if applicable.
OIG/SAM Exclusion Verification: Confirmation that the provider is not excluded from federal programs.
Previous Privileges: Documentation of prior hospital privileges and scope of practice.
Internal Review Controls
Hospitals implement internal review controls to ensure the privileging process is consistent and compliant:
Peer Review Committees: Assess clinical competence and specialty-specific skills.
Medical Staff Oversight: Bylaws define authority for approving, revising, or limiting privileges.
Periodic Re-Privileging: Most hospitals re-evaluate practitioners every 24 months to confirm ongoing competence.
Documentation Audits: Random and scheduled audits verify the accuracy of submitted records.
Governing Body Approval: Final authorization of privileges rests with the hospital’s governing body to comply with CMS CoPs.
Continuous Monitoring: Performance, outcomes, and patient feedback are reviewed to identify potential limitations or additional training needs.
Revenue, Compliance, and Risk Impact
Hospital privileging affects revenue, compliance, and risk management. Proper privileging minimizes claim denials, legal exposure, and ensures safe patient care.
Billing and Claims Risk
Incomplete privileging makes direct billing challenging. Insurers may reject claims if procedures are performed by doctors who do not have active privileges. These denials cause delays in revenue collection and increase administrative workload.
Ongoing monitoring and documentation of privileges reduces delays. Hospitals that maintain accurate privileging records can prevent up to 7% of annual revenue losses tied to rejected claims. Routine verification also strengthens audit readiness and payer trust.
Legal and Compliance Exposure
Failure to follow privileging protocols increases regulatory risk. Hospitals may face CMS dues, state sanctions, or even loss of Medicare and Medicaid participation for noncompliance. Legal exposure increases when providers operate beyond granted privileges.
Regular audits, peer reviews, and re-privileging reduce these risks. Reporting limitations, suspensions, or revocations to NPDB and state authorities ensures compliance. Strong privileging systems protect both patients and the hospital from liability.
Conclusion
Proper hospital privileging ensures providers deliver care within verified competencies while supporting patient safety, regulatory compliance, and operational efficiency. Hospitals that maintain clear privileging workflows reduce claim denials, legal exposure, and administrative delays.
Continuous monitoring, periodic re-privileging, and accurate documentation protect both patients and institutions. Understanding the hospital privileging process, requirements, and oversight responsibilities allows healthcare teams to optimize performance, revenue, and compliance outcomes effectively.
FAQs
What is the Hospital Privileging Process?
The Hospital Privileging Process defines the clinical procedures a provider is authorized to perform within a facility. It ensures patient safety, regulatory compliance, and an appropriate scope of practice.
How does privileging differ from credentialing?
Credentialing verifies a provider’s qualifications, licensure, and education. Privileging authorizes specific procedures based on verified competencies.
What are the core requirements for hospital privileges?
Providers must submit verified licenses, board certifications, clinical experience, professional references, and malpractice history. Hospitals may also assess competency through peer review.
Why is ongoing monitoring important in privileging?
Continuous monitoring ensures providers maintain skills, comply with regulations, and deliver safe patient care. It prevents expired privileges from affecting billing or clinical quality.
How does privileging impact revenue and compliance?
Incomplete or outdated privileges can cause claim denials and legal exposure. Proper privileging safeguards revenue, audit readiness, and adherence to CMS and state requirements.





