When healthcare providers, administrators, and billing specialists visit this blog, they often face a common challenge: understanding the difference between credentialing and enrollment. Confusing the two can cause delays in patient care, payment issues, and operational inefficiencies. In 2026, enrollment challenges and credentialing delays can result in 25-50% claim delays, costing some businesses over $1 million per year. Have you ever thought about how much these delays could be affecting your practice’s revenue and compliance?
Healthcare organizations are also contending with longer processing times and staffing pressures. The average credentialing process now takes 90–120 days, and enrollment can take 90–180 days, often extended by missing documentation or payer-specific rules. With 85% of applications containing errors, practices must prioritize accurate, complete submissions to maintain revenue flow and patient access.
This guide explains credentialing vs enrollment, the role each process plays, and how they affect provider billing and network participation. You will learn how credentialing verifies provider qualifications, how enrollment allows claim submission, and why understanding both processes helps prevent revenue delays and compliance risks.
Credentialing vs Enrollment
Credentialing and enrollment are core processes that determine whether a provider can deliver services and receive payment from insurance networks.
Understanding the distinction helps healthcare organizations maintain compliance, avoid claim denials, and ensure proper reimbursement.
What Is Provider Credentialing?
Provider credentialing is the verification process used to confirm a healthcare professional’s qualifications and professional background before participation in healthcare networks.
Key elements reviewed during credentialing include:
- Medical education and training history
- State licensure verification
- Board certification status
- DEA registration
- Work history and clinical experience
- Malpractice insurance coverage
- Malpractice claims history
- Professional references
What Is Provider Enrollment?
Provider enrollment is the administrative process that registers a healthcare provider with an insurance payer so the provider can bill and receive payment for services.
Enrollment requires submitting provider and practice data to insurance networks such as:
- Medicare
- Medicaid
- Commercial insurers
- Regional health plans
Information typically submitted during enrollment includes:
- National Provider Identifier (NPI)
- Tax Identification Number (TIN)
- Practice location and contact details
- W-9 documentation
- Banking information for electronic payments
- Malpractice insurance verification
The Difference Between Credentialing and Enrollment
Short Description: Understanding the distinction between credentialing and enrollment is essential for healthcare providers and administrators. Both processes impact provider participation, billing, and compliance.
Purpose of Each Process
Provider Credentialing: Verifies a provider’s qualifications, licenses, education, training, and professional history. It ensures providers meet regulatory, safety, and quality standards. In 2026, over 85% of healthcare organizations report credentialing errors as a top cause of claim delays.
Provider Enrollment: Registers a provider with insurance networks to enable reimbursement for services. Enrollment secures network access and ensures patients can use insurance coverage for in-network care.
Who Performs the Process
Credentialing: Conducted by healthcare organizations, hospitals, or credentialing verification organizations (CVOs). Delegated credentialing allows trusted third parties to perform credentialing for multiple payers.
Enrollment: Primarily handled by the provider or administrative staff. Some payers require direct submissions, while others accept enrollment through centralized platforms like CAQH.
Documentation Requirements
Credentialing: Requires proof of licensure, education transcripts, board certifications, DEA registration, malpractice history, professional references, and career history.
Enrollment: Requires provider demographic information, practice location, Tax Identification Number (TIN), insurance contracts, and verification of licensure and malpractice coverage.
Impact on Provider Participation
1. Credentialing confirms the provider is eligible to deliver services, impacting hiring, privileging, and compliance with state and federal regulations.
2. Enrollment determines which insurance networks a provider can participate in. Providers cannot see patients in-network without completed enrollment.
Effect on Billing and Reimbursement
1. Credentialing ensures the provider meets standards to bill services, protecting against denials due to ineligible providers.
2. Enrollment ensures that claims are submitted to payers correctly and reimbursed. In 2026, practices with incomplete enrollment see up to 40% of claims denied for administrative reasons.
Credentialing vs Enrollment in the Healthcare Revenue Cycle
Credentialing and enrollment are critical steps in healthcare revenue cycle management. Understanding their roles helps providers maintain compliance and secure timely reimbursements.
How Credentialing Supports Compliance
Credentialing ensures healthcare providers meet all legal, professional, and payer-specific standards before delivering care. It verifies education, licensure, board certifications, malpractice history, and professional affiliations. Proper credentialing reduces compliance risks, protects patient safety, and strengthens the provider’s standing with insurance networks.
Key points for compliance support:
- Verify provider licensure, DEA registration, and board certifications.
- Check professional references, malpractice claims, and disciplinary actions.
- Maintain records for re-credentialing every 3–5 years.
- Reduce risks of fraud, abuse, and claim denials.
- Enhance trust with insurers and patients.
How Enrollment Enables Claim Submission
Provider enrollment allows healthcare providers to register with insurance networks, making them eligible to submit claims for services rendered. The enrollment process requires practice details, TIN, malpractice coverage, and proof of licensure. In 2026, enrollment timelines range between 90 and 180 days, depending on the payer and state regulations. Incomplete enrollment can delay payments and limit patient access to in-network care.
Key points for claim submission:
- Submit provider details and required documentation to payers.
- Confirm contracts with commercial insurers, Medicare, and Medicaid.
- Use centralized databases such as CAQH or NCQA to streamline applications.
- Ensure data accuracy to prevent claim denials.
Financial Risks of Incomplete Enrollment
Incomplete enrollment exposes healthcare organizations to significant revenue risks. Providers without approved enrollment cannot bill insurers, resulting in lost income and delayed reimbursements. In 2026, up to 40% of denied claims are associated with missing enrollment or credentialing information. Financial losses can also affect patient satisfaction if services are blocked due to out-of-network status.
Key points on financial risks:
- Delayed claim payments due to missing payer approvals.
- Retroactive billing challenges and administrative burdens.
- Increased denials and resubmissions of claims.
- Risk of patient dissatisfaction and reduced access to care.
- Maintaining updated enrollment and credentialing files minimizes revenue loss.
Credentialing Process for Healthcare Providers
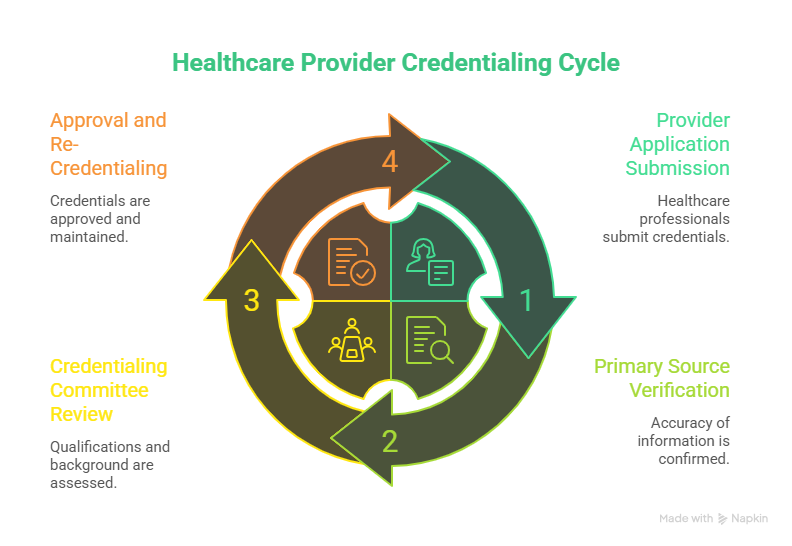
The credentialing process ensures that healthcare providers meet all professional, legal, and payer requirements before delivering patient care. This section explains each step, from application submission to re-credentialing, highlighting how accurate credentialing protects organizations from compliance and financial risks.
Provider Application Submission
Provider credentialing begins with submitting a complete application. This includes personal, professional, and practice-related information needed by insurers or credentialing committees.
Key points:
- Include licensure, DEA registration, and board certifications.
- Provide education and training details, along with professional affiliations.
- Include malpractice history and disciplinary actions.
- Submit practice addresses, NPI, and Tax Identification Number (TIN).
- Ensure all documents are current and verifiable.
Primary Source Verification
Primary Source Verification (PSV) confirms that all provider information is accurate and authentic. Organizations verify each detail with sources to avoid fraud and ensure compliance.
Key points:
- Contact licensing boards and educational institutions directly.
- Confirm DEA registration and professional certifications.
- Verify malpractice claims and work history.
- Review any disciplinary or legal actions reported against the provider.
- Maintain a digital or physical file for audit purposes.
Credentialing Committee Review
Once verification is complete, a credentialing committee evaluates the provider’s qualifications against organizational and payer standards. This review ensures only qualified providers are approved.
Key points:
- The committee includes clinical leaders and compliance officers.
- Assess the provider’s training, experience, and professional history.
- Compare documentation with regulatory and payer standards.
- Approve or request additional documentation if required.
- Document the committee’s decision for record-keeping.
Approval and Re-Credentialing Cycle
After approval, providers are added to the approved roster. Re-credentialing occurs every 3–5 years to maintain compliance and verify updated provider information.
Key points:
- Monitor license renewals and certifications continuously.
- Update malpractice claims and disciplinary records as needed.
- Schedule re-credentialing notifications before expiration.
- Ensure timely submission to avoid delays in network participation.
- Maintain accurate records to reduce claim denials and audit risks.
Payer Credentialing vs Enrollment
Payer credentialing and enrollment are two distinct steps for provider participation in insurance networks. This section explains how insurance companies verify credentials and finalize network participation, highlighting their impact on claims and reimbursements.
How Insurance Companies Conduct Credentialing
Insurance companies perform credentialing to confirm a provider’s qualifications and compliance before approving network participation. This step protects payers from fraud and ensures patient safety.
Key points:
- Review provider licensure, DEA registration, and board certifications.
- Verify education, training, and work history through primary sources.
- Examine malpractice claims, disciplinary actions, and sanctions.
- Confirm provider meets payer-specific clinical and quality standards.
- Use databases like CAQH ProView and NCQA standards to streamline verification.
How Payer Enrollment Finalizes Network Participation
Once credentialing is complete, payer enrollment authorizes the provider to participate in the network and receive reimbursement for services rendered. This step ensures the provider can bill insurance correctly.
Key points:
- Submit enrollment forms with verified provider information.
- Negotiate contracts and define reimbursement terms if applicable.
- Receive network approval or denial; approval allows claims submission.
- Ensure accurate NPI, Tax ID, and practice location for billing purposes.
- Maintain updated enrollment records to prevent claim delays or denials.
Medical Credentialing vs Payer Enrollment Requirements
Medical credentialing and payer enrollment have distinct documentation requirements. Understanding these differences ensures providers meet compliance standards and receive timely reimbursement.
Key Documentation for Credentialing
Credentialing verifies a provider’s qualifications and professional history to participate safely in healthcare services.
Essential documents include:
- Provider licensure and DEA registration.
- Board certifications and specialty credentials.
- Education and training records from primary sources.
- Professional references and work history verification.
- Malpractice insurance and claims history.
- Criminal background and sanctions disclosure.
Key Documentation for Enrollment
Payer enrollment ensures providers can bill the insurance network and receive reimbursement for services rendered.
Critical documents include:
- Completed payer enrollment forms.
- Provider NPI and Tax Identification Number (TIN).
- Practice location details and hours of operation.
- Proof of malpractice insurance coverage.
- Any contracts or agreements required by the payer.
- Updated CAQH or payer-specific data submissions.
Credentialing vs Enrollment: Key Differences Table
This table summarizes the main distinctions between credentialing and enrollment, helping healthcare providers and billing teams understand each process and its impact on network participation and reimbursement.
| Aspect | Credentialing | Enrollment |
| Purpose | Verifies provider qualifications and eligibility to deliver care | Registers provider with insurance networks for reimbursement |
| Performed By | Healthcare organizations, insurance CVOs, and credentialing committees | Providers submitting to insurance networks or payers |
| Required Documentation | Licenses, certifications, education, training, work history, references, malpractice history | Enrollment forms, NPI, TIN, practice location, insurance coverage, payer-specific agreements |
| Timeline | Several weeks are often required before enrollment | Several weeks to months; starts after credentialing approval |
| Outcome | Confirms competency and compliance with professional standards | Authorizes the provider to bill and receive payment from payers |
| Impact | Ensures patient safety, provider legitimacy, and regulatory compliance | Enables claims submission, revenue generation, and patient access |
Conclusion
Understanding credentialing vs enrollment is critical for healthcare providers, administrators, and billing specialists. Accurate credentialing verifies provider qualifications, while proper enrollment ensures timely reimbursement and network participation. Both processes directly impact compliance, revenue, and patient access.
Healthcare businesses can reduce claim denials and financial risk by maintaining accurate documents and following payer and regulatory standards. Keeping up with current standards in 2026 enables providers to protect revenue, boost operational efficiency, and ensure patient care.
FAQs
What is the difference between credentialing and enrollment?
Credentialing verifies a provider’s qualifications and history, while enrollment registers them with insurance networks to submit claims.
How long does the credentialing process take?
In 2026, credentialing typically takes 90–120 days, depending on provider documentation and organizational review.
Why is payer enrollment important for providers?
Enrollment allows providers to bill insurers, receive reimbursement, and ensure patients can access in-network care.
What documents are needed for credentialing?
Providers need licenses, board certifications, education records, work history, professional references, and malpractice claims history.
What happens if enrollment is incomplete?
Incomplete enrollment can cause claim denials, delayed payments, and lost revenue, affecting both the practice and patient access.





