Healthcare organizations face growing pressure to maintain accurate provider data at all times. What happens if a provider’s license is suspended today, but your system only checks credentials once a year? Delays in identifying license issues, sanctions, or network changes can result in claim denials, compliance penalties, and network suspensions. Many organizations still rely on periodic credentialing, which leaves gaps between verification cycles.
The Continuous Provider Monitoring Standards 2026 bridge this gap by moving from scheduled tests to ongoing validation. NCQA updates effective July 2025 and extending into 2026 emphasize more frequent oversight of provider credentials and data. Industry guidance also indicates that licensure and sanctions must be reviewed at least every 30 days, rather than annually. This shift directly impacts medical coders, billing teams, and compliance officers who depend on accurate provider data.
This blog explains how continuous monitoring improves compliance, reduces risk, and supports accurate billing and credentialing workflows. Many healthcare groups rely on healthcare credentialing services to maintain provider accuracy and compliance. It also highlights the risks of outdated methods, which can trigger downstream issues such as claim rejections and insurance network suspensions. The focus is on aligning operational processes with real-time verification standards required in 2026.
Continuous provider monitoring standards 2026
This section explains how provider monitoring has shifted from periodic reviews to continuous validation. It focuses on regulatory changes, system requirements, and risks linked to outdated credentialing.
What does Continuous Provider Monitoring Mean
Continuous monitoring replaces fixed review cycles with ongoing verification of provider data. Many organizations strengthen this process through professional Physician Credentialing Services that keep provider records current and verified. It includes real-time checks for licenses, sanctions, and certifications.
- Data is checked daily or in real time.
- Updates reflect immediately across systems.
- Errors are identified without waiting for audit cycles.
- Reduces reliance on spreadsheets and manual tracking
A key expectation in 2026 is NCQA real-time license verification. This ensures provider status is confirmed directly from issuing authorities. It reduces delays and improves accuracy in credentialing records.
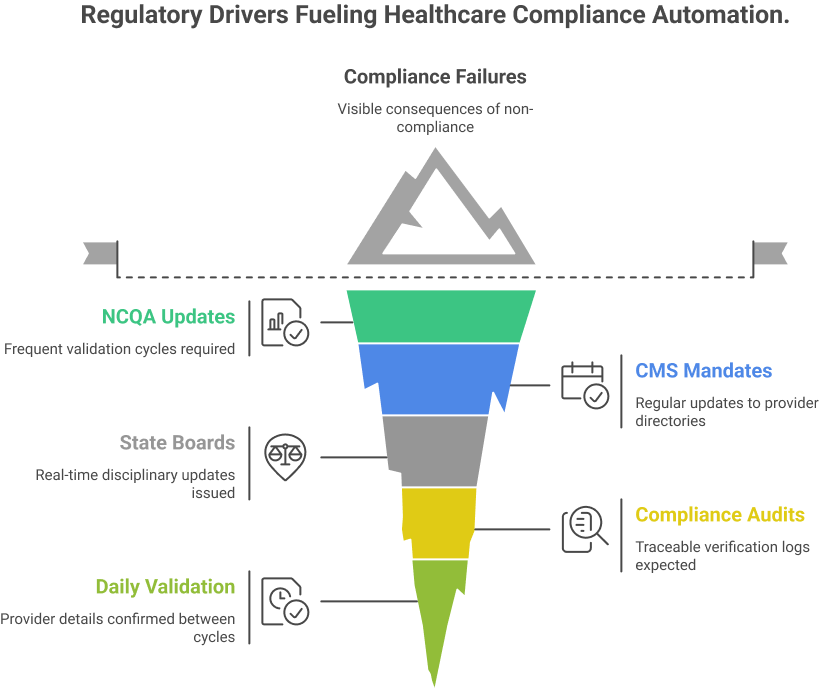
Regulatory Drivers Behind the Shift
Regulatory bodies are pushing continuous oversight to reduce compliance failures.
- NCQA updates now require frequent validation cycles
- CMS mandates regular updates to provider directories
- State boards issue real-time disciplinary updates
- Compliance audits expect traceable verification logs.
A major update is the move to daily provider data validation. Organizations must confirm that provider details remain accurate between billing and reporting cycles.
Failure to meet these expectations can lead to:
- Insurance network suspensions
- Claim rejections
- Regulatory penalties
This shift forces healthcare systems to move away from periodic checks and adopt 2026 healthcare compliance automation to remain compliant.
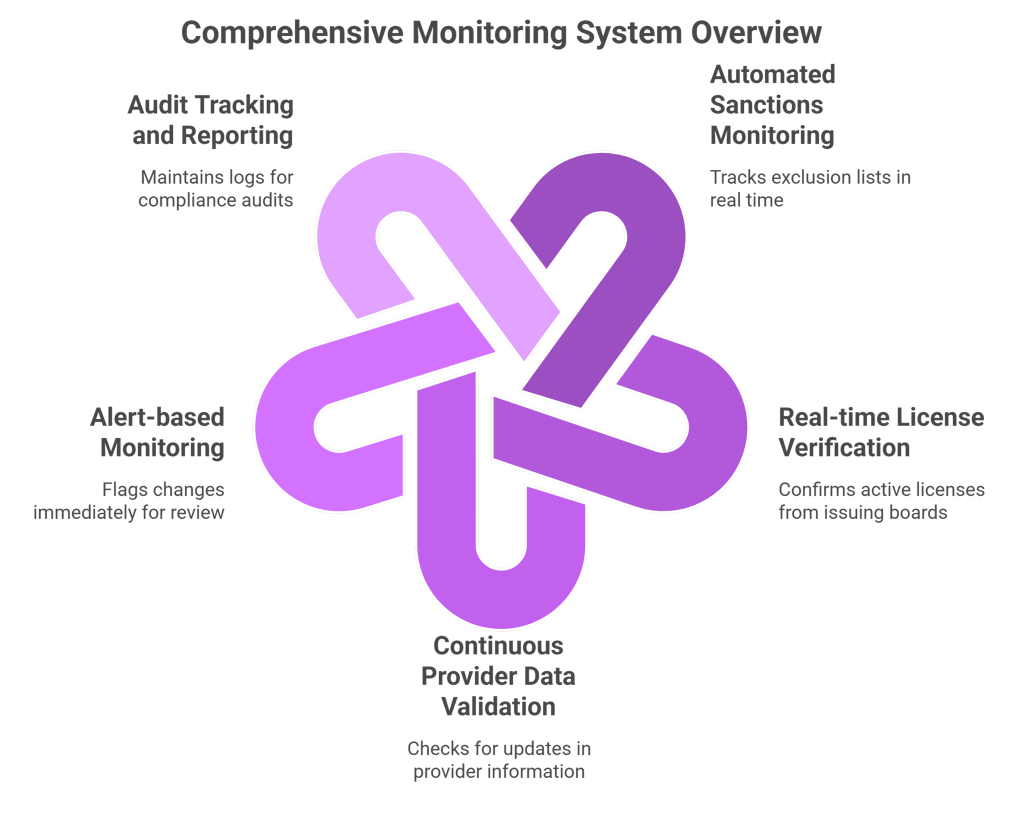
Key Elements of a Monitoring System
A compliant monitoring system must include structured, automated controls.
- Automated sanctions monitoring for medical practices
Tracks exclusion lists such as OIG and SAM databases in real time.
- Real-time license verification
Confirms active licenses directly from issuing boards
- Continuous provider data validation
Checks updates for address, specialty, and network participation
- Alert-based monitoring
Flags change immediately for review and action.
- Audit tracking and reporting
Maintains logs for compliance audits and regulatory checks
Moving from Manual to Automated Monitoring
Continuous provider monitoring standards 2026 require a shift from manual credential checks to real-time tracking. Traditional cycles cannot detect mid-cycle changes. Automation now drives compliance, reduces exposure, and supports payer expectations.
Risks of Periodic Credentialing
Periodic credentialing creates gaps between review cycles. These gaps expose healthcare organizations to compliance and financial risks.
Key risks include:
1. Delayed detection of license sanctions or expirations
2. Increased chance of billing with inactive providers
3. Retroactive payer audits and recoupments
4. Network suspension due to late updates
5. Administrative burden on credentialing teams
Real-Time “Continuous Monitoring” vs Periodic Credentialing
Continuous monitoring replaces fixed intervals with ongoing checks. This aligns with payer and NCQA expectations for active compliance tracking.
| Category | Periodic Credentialing | Continuous Monitoring |
| Monitoring frequency | Every 12–24 months | Daily or real-time updates |
| Risk detection | Delayed identification | Immediate alerts on changes |
| Data accuracy | Snapshot-based | Always current |
| Compliance response | Reactive | Proactive |
NCQA Real-Time License Verification
National Committee for Quality Assurance now supports real-time license verification as part of modern credentialing standards.
This approach validates provider data against primary sources on an ongoing basis.
Core elements include:
- Daily license status checks with state boards
- Continuous monitoring of exclusions and sanctions
- Real-time updates to provider profiles
- Alerts for contract-impacting changes
Operational Impact for Healthcare Roles
Continuous monitoring affects multiple roles across healthcare organizations. It changes workflows and accountability.
Impact by role:
1. Medical Coders and Billers
- Avoid claims tied to inactive providers
- Reduce denial risk
2. Credentialing Specialists
- Shift from periodic reviews to monitoring alerts
- Maintain updated provider files
3. Practice Managers
- Ensure uninterrupted payer participation
- Monitor compliance dashboards
4. Revenue Cycle Teams
- Prevent revenue loss from suspended providers
- Improve claim acceptance rates
5. Compliance Officers
- Track sanctions and regulatory changes
- Reduce audit exposure
Automated Sanctions Monitoring for Medical Practice
Automated sanctions monitoring tracks provider exclusions, disciplinary actions, and license issues in real time. These provider monitoring standards require active tracking instead of periodic reviews.
This section explains why sanctions monitoring matters and where the data comes from. It supports compliance, billing accuracy, and network participation.
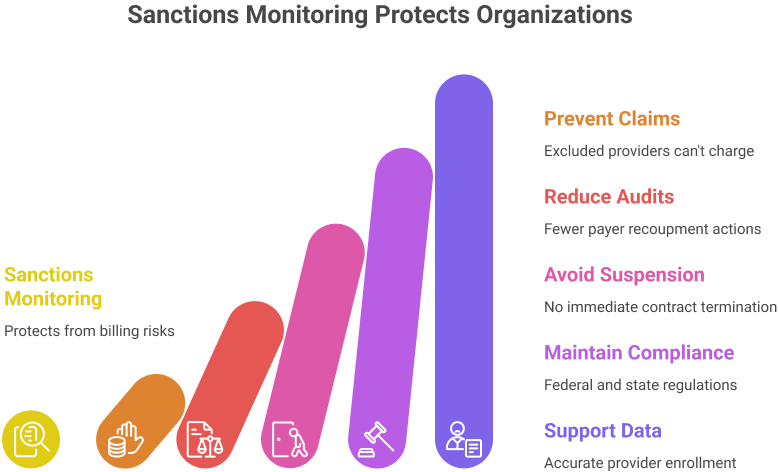
Why Sanctions Monitoring Matters
Sanctions monitoring protects organizations from billing and compliance risks. Without it, providers with restrictions may continue to charge, which leads to serious issues.
Key reasons include:
1. Prevent claims tied to excluded or restricted providers
2. Reduce payer audits and recoupment actions
3. Avoid immediate contract suspension by payers
4. Maintain compliance with federal and state regulations
5. Support accurate provider enrollment data
Under the continuous provider monitoring standards 2026, delayed detection is a major risk. A flagged provider can affect claims and contracts within days.
Key Monitoring Sources
Effective sanctions monitoring depends on reliable data sources. These sources provide updates on provider status across regulatory bodies.
Primary monitoring sources include:
National Practitioner Data Bank
- Tracks malpractice payments and adverse actions
Office of Inspector General
- Maintains exclusion lists for federal programs
State licensing boards
- Provide license status updates and disciplinary actions.
System for Award Management
- Lists excluded entities and individuals.
Payer-specific exclusion lists
- Track providers removed from networks
Daily Provider Data Validation and Compliance Automation
Daily provider data validation ensures that all provider records remain current across payer and regulatory systems. Continuous provider monitoring standards 2026 require ongoing checks instead of periodic updates.
Compliance automation supports real-time updates, reduces manual work, and strengthens oversight. This section focuses on what needs daily validation and how automation supports compliance.
What Needs Daily Validation
Healthcare organizations must validate key provider data daily to stay compliant and avoid disruptions. Static data is no longer acceptable under current monitoring expectations.
Critical data points include:
- License status and expiration dates
- Sanctions and exclusion list status
- DEA registration and certification updates
- Provider demographics and practice locations
- Network participation status with payers
A delay in updating any of these can trigger billing issues or contract actions. If a state board updates a license on a weekday, payer systems may react within a short time frame.
Role of Compliance Automation
Compliance automation replaces manual tracking systems with real-time monitoring tools. It supports daily provider data validation and improves response time.
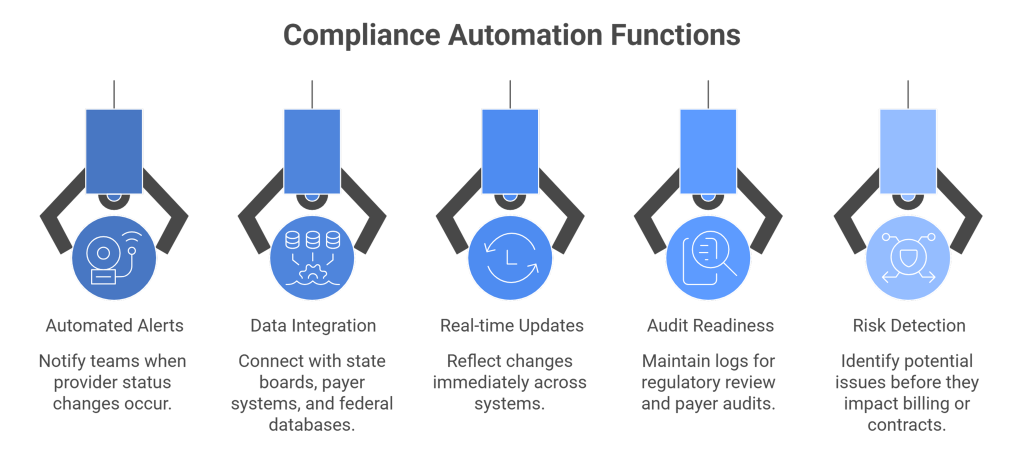
Key functions include:
Automated alerts
Notify teams when provider status changes occur
Integration with data sources
Connect with state boards, payer systems, and federal databases.
Real-time updates
Reflect changes immediately across systems.
Audit readiness
Maintain logs for regulatory review and payer audits.
Risk detection
Identify potential issues before they impact billing or contracts.
Avoiding Insurance Network Suspensions
Insurance network suspensions can occur quickly when provider data is outdated or non-compliant. Continuous provider monitoring standards 2026 require ongoing tracking to reduce this risk.
This section explains key causes of suspension and how continuous monitoring helps prevent disruptions in payer participation and claims processing.
Common Causes of Suspension
Network suspensions usually occur due to gaps in provider oversight or delayed updates. These issues are often preventable with proper monitoring.
Common causes include:
- Expired or inactive medical licenses
- Provider exclusion from federal programs
- Failure to report changes in practice status
- Delayed updates in payer credentialing systems
- Sanctions from state or federal authorities
Avoiding Insurance Network Suspensions
Insurance network suspensions can occur quickly when provider data is outdated or non-compliant. Continuous provider monitoring standards 2026 require ongoing tracking to reduce this risk.
This section explains key causes of suspension and how continuous monitoring helps prevent disruptions in payer participation and claims processing.
Common Causes of Suspension
Network suspensions usually occur due to gaps in provider oversight or delayed updates. These issues are often preventable with proper monitoring.
Common causes include:
- Expired or inactive medical licenses
- Provider exclusion from federal programs
- Failure to report changes in practice status
- Delayed updates in payer credentialing systems
- Sanctions from state or federal authorities
Prevention Through Monitoring
Continuous monitoring reduces the risk of suspension by identifying issues early. It replaces periodic checks with real-time oversight.
Key prevention steps include:
1. Daily license verification
Ensure providers maintain active and valid credentials
2. Real-time sanction monitoring
Track updates from the Office of Inspector General and other sources
3. Integration with payer systems
Keep enrollment data aligned with network requirements
4. Automated alerts and notifications
Respond quickly to status changes
5. Routine data validation
Maintain accurate provider records across all systems
Implementation Framework for 2026 Continuous provider monitoring standards 2026
Adopting continuous provider monitoring standards 2026 requires a structured shift from manual workflows to real-time systems. Most organizations fail due to a lack of a clear implementation path.
This section outlines a step-by-step approach and the tools required to support daily monitoring, compliance, and accurate provider data management.
Step-by-Step Approach
A structured plan reduces risk and supports a smooth transition to continuous monitoring. Each step must align with compliance and operational needs.
Key steps include:
1. Assess the current credentialing process
- Identify gaps in periodic tracking systems
- Review data sources and update cycles
2. Define monitoring requirements
- Set rules for license, sanctions, and exclusion checks
- Align with payer and regulatory expectations
3. Centralize provider data
- Create a single source of truth
- Remove duplicate or outdated records
4. Integrate real-time monitoring
- Connect to state boards and federal databases
- Enable continuous alerts for changes
5. Establish response protocols
- Define actions for flagged providers
- Assign roles for compliance and billing teams
6. Audit and refine regularly
- Review system performance
- Update processes based on regulatory changes
Tools and Systems Required
Technology plays a central role in supporting continuous monitoring. Manual systems cannot meet real-time compliance needs.
Essential tools include:
1. Credentialing and enrollment platforms
Maintain provider data and track updates across systems
2. Automated monitoring solutions
Provide real-time alerts for sanctions and license changes
3. Integration with external data sources
Connect to systems like the National Practitioner Data Bank and state licensing boards
4. Compliance management systems
Track regulatory requirements and audit readiness
5. Reporting and analytics tools
Monitor trends, risks, and compliance status
Conclusion
Continuous provider monitoring standards 2026 require a shift from periodic checks to real-time validation. Healthcare organizations must adopt automated systems to detect license changes, sanctions, and exclusions without delay. This reduces compliance gaps and supports accurate billing and network participation.
Manual credentialing creates avoidable risks in today’s regulatory environment. Aligning with NCQA real-time license verification and daily provider data validation helps prevent insurance network suspensions and protects revenue integrity. Continuous monitoring is now a core requirement for compliance, not an optional upgrade.
FAQs
What are the Continuous Provider Monitoring Standards 2026?
They require real-time, ongoing verification of provider licenses, sanctions, and credentials instead of periodic reviews. This ensures accurate data and supports compliance with payer and regulatory expectations.
Why is periodic credentialing considered a risk in 2026?
Periodic credentialing leaves gaps between review cycles, allowing license issues or sanctions to go unnoticed. These delays can lead to claim denials, audits, and insurance network suspensions.
What is NCQA’s real-time license verification?
The National Committee for Quality Assurance’s real-time license verification continuously checks provider credentials against primary sources. It improves accuracy and reduces delays in identifying compliance issues.
How does continuous monitoring help prevent insurance network suspensions?
It provides instant alerts on provider status changes, allowing immediate action before payers respond. This reduces the risk of suspension due to outdated or incorrect provider data.
Which tools support the Continuous Provider Monitoring Standards 2026?
Automated monitoring systems, credentialing platforms, and compliance tools support real-time validation and tracking. Integration with sources like the Office of Inspector General ensures accurate sanctions and license monitoring.





