Have you ever considered how a single Medicaid denial in one state may affect your entire Medicare and CHIP enrollment nationally? For healthcare providers, medical billers, and credentialing specialists, the 2026 CMS enforcement rules turn even minor compliance errors into major operational and financial risks. Recent CMS enforcement actions in early 2026 show major plan sponsors, including Elevance Health, Inc. and Aspirus Health Plan, Inc., facing enrollment suspensions and terminations, highlighting the nationwide reach of these rules.
Understanding CMS cross‑program termination enforcement is no longer optional for organizations that rely on federal and state reimbursements. CMS has shifted its enforcement strategy in 2026 from a “best-effort” compliance model to strict real-time accountability. Providers whose internal records do not align precisely with federal enrollment databases risk audits, claim denials, and immediate termination under the new rules.
This guide breaks down how a single compliance error can cascade across Medicare, Medicaid, and CHIP enrollments. It explains enforcement triggers, financial and operational impacts, and the steps coders, credentialers, and billing teams must take to protect their practices. You will also find actionable strategies to appeal cross-program enrollment bans before they escalate.
What Is CMS Cross-Program Termination Enforcement
CMS cross-program termination enforcement ensures that if a provider is terminated from one federal or state program, they are automatically removed from all other CMS programs nationwide. This rule, effective in 2026, creates a “domino effect,” meaning a single state Medicaid termination now triggers automatic termination from Medicare and CHIP across all states.
Definition and Regulatory Basis
CMS cross-program termination enforcement stems from federal regulations codified under 42 CFR Part 455 and program integrity updates released in early 2026. The rule links Medicaid, Medicare, and CHIP enrollments to prevent providers who are terminated for cause in one program from continuing participation in others. CMS reported that in Q1 2026, over 1,250 providers faced cross-program terminations due to non-compliance in a single state program, emphasizing the scope of enforcement. Providers must now comply with all program integrity standards, including updated healthcare provider exclusion screening 2026 protocols.
Why CMS Enforces Cross-Program Termination
The policy protects federal funds and ensures program integrity by reducing fraud, waste, and abuse. Linking state terminations to national enrollment prevents providers with compliance issues from continuing to bill Medicare or CHIP. While the rule strengthens oversight, it also increases multistate provider enrollment risk, as a single administrative or documentation error can jeopardize nationwide practice operations. Providers and billing teams must remain vigilant, understand the automatic linkage, and maintain precise documentation to reduce the risk of appeals for a cross-program enrollment ban.
The Domino Effect: Medicaid to Medicare Termination Linkage
CMS cross-program termination enforcement creates a national chain reaction when a provider is terminated from one program. Understanding this “domino effect” is critical for providers and billing teams to avoid sudden nationwide enrollment loss.
Step-by-Step Enforcement Chain
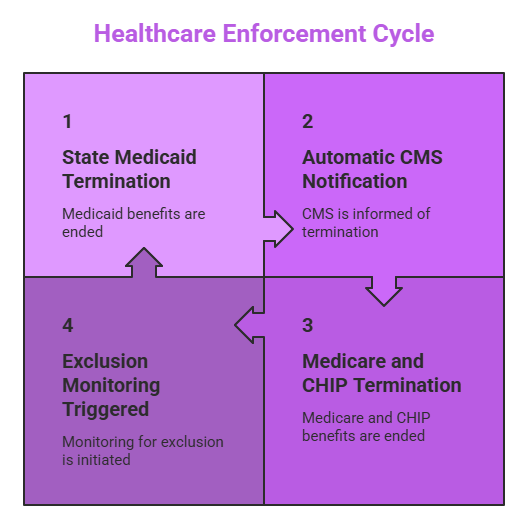
The 2026 rule follows a structured enforcement sequence:
1. State Medicaid Termination: A provider with compliance issues or documentation errors in one state Medicaid program is terminated.
2. Automatic CMS Notification: CMS receives real-time updates from state Medicaid programs as part of updated CMS program integrity updates.
3. Medicare and CHIP Termination: The provider is automatically removed from all other programs, including Medicare and CHIP, across every state.
4. Exclusion Monitoring Triggered: This enforces healthcare provider exclusion screening in 2026, preventing billing until issues are resolved.
Multi-State Enrollment Risk
Providers with multiple practice locations face heightened exposure. Each state program’s compliance requirements differ slightly, which increases the multistate provider enrollment risk. Key points to manage risk:
- Maintain accurate provider documentation across all states.
- Track and update state-specific Medicaid enrollment deadlines.
- Monitor CMS and state program communications regularly.
Key Triggers of Cross-Program Termination
CMS cross-program termination enforcement is activated when specific compliance failures occur. Recognizing these triggers helps providers prevent abrupt termination across Medicare, Medicaid, and CHIP.
Exclusion Screening Failures
Providers must comply with the healthcare provider exclusion screening requirements of 2026. Failure to check federal and state exclusion lists can lead to automatic CMS cross-program termination enforcement. Even minor oversights, such as an expired license or delayed update, can remove a provider from all programs nationwide.
- OIG and state-level exclusion checks must be conducted monthly.
- Providers listed for fraud, abuse, or patient harm are automatically terminated across all programs.
- Over 900 providers in 2026 were terminated due to incomplete exclusion updates.
Maintaining real-time monitoring of provider status is critical. Many healthcare organizations use Healthcare Audit Protection Services to strengthen compliance oversight and reduce termination risk. Credentialing and compliance teams must ensure that all providers are actively screened and any discrepancies are resolved immediately. Automated tools can reduce manual errors, but do not replace human verification.
- Use centralized exclusion dashboards to track updates.
- Document all exclusion screenings for audit purposes.
- Educate staff on changes to federal or state exclusion databases.
Credentialing and Enrollment Errors
Errors in enrollment applications or incomplete documentation can trigger a cross-program termination cascade. CMS now links state Medicaid enrollment to Medicare and CHIP, meaning one mistake in a single state can jeopardize national enrollment.
- Verify all provider credentials, licenses, and NPIs across states.
- Ensure addresses, specialty, and practice location are accurate in all systems.
- Update enrollment data immediately after changes occur.
Proactive oversight is essential to reduce multistate provider enrollment risk. Many providers rely on Physician Credentialing Services to keep records accurate across state and federal systems. Credentialing teams should implement regular audits and cross-checks to detect missing forms or incorrect entries before submission to CMS.
- Maintain a checklist for every state application.
- Conduct quarterly internal reviews of provider enrollment data.
- Train staff to recognize common errors that lead to terminations.
Coding and Billing Violations
Improper coding or billing can trigger program integrity reviews, which may result in cross-program termination. CMS audits identify discrepancies in claim submission, documentation, and adherence to NCCI edits.
- Ensure all claims are supported by proper documentation.
- Follow Medicare, Medicaid, and CHIP coding rules consistently.
- Monitor for common errors such as duplicate billing or unbundled procedures.
Recent 2026 data show that 25% of terminations across programs were linked to coding or billing violations. Revenue cycle teams must monitor claims proactively to prevent escalations. Implementing standardized audits and real-time compliance checks minimizes the risk of nationwide termination.
- Perform routine internal coding audits.
- Provide ongoing training for coders and billing staff.
- Keep updated with CMS program integrity updates and policy changes.
Financial and Operational Impact on Healthcare Organizations
The 2026 CMS cross-program termination enforcement can have serious financial and operational consequences. Understanding these risks helps healthcare leaders prepare and protect their practice from nationwide disruptions.
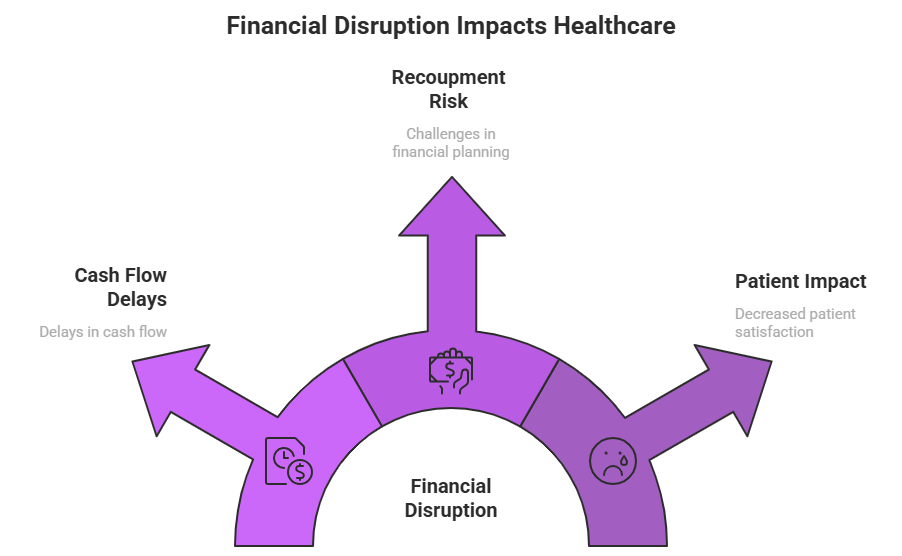
Revenue Cycle Disruption
CMS cross-program termination enforcement can immediately halt reimbursements from Medicare, Medicaid, and CHIP. This creates a direct cash flow disruption that affects daily operations, payroll, and vendor payments.
Billing teams must quickly identify which providers are impacted and adjust claims submission workflows. Practices should pause claims for terminated providers and use enrollment dashboards to track real-time status.
- Claims submitted after termination are automatically rejected.
- Accounts receivable can grow rapidly.
- Coordination between billing and credentialing is essential.
Retroactive Recoupment Risk
CMS may recover payments for claims submitted while a provider’s enrollment was invalid. Retroactive recoupments can include multiple months or even years of claims, heavily impacting financial reserves.
Preventing recoupments requires proactive audits and verifying provider status before each claim submission. Maintaining updated credentialing records and documenting all communications with CMS is critical.
- Conduct monthly reconciliation of claims against enrollment status.
- Train staff to flag high-risk claims.
- Keep detailed records for all provider status changes.
Patient and Practice Impact
Cross-program terminations affect both patient care and practice operations. Patients may face delays, service denials, or confusion regarding coverage while administrative staff manages enforcement issues.
Practices should develop contingency plans to ensure continuity of care. Clear communication with patients and internal teams, along with temporary billing adjustments, minimizes disruptions and protects practice reputation.
- Notify patients proactively about potential coverage changes.
- Dedicate staff to manage termination and reinstatement.
- Review workflows to maintain consistent patient care.
How to prevent cross‑program termination: CMS cross‑program termination enforcement
Practical steps now can stop a single error from triggering nationwide termination. This section gives two high‑impact controls your teams can apply immediately. The focus is on daily, monthly, and system‑level checks that keep enrollment and billing aligned with CMS expectations.
Monthly Exclusion Screening
Regular exclusion checks are essential to prevent cross-program termination. Missing or delayed screening of federal or state databases can trigger automatic removal from Medicare, Medicaid, and CHIP.
Teams should review alerts immediately and document all actions, including staff and date. Automation can flag potential issues, but human review ensures timely resolution before enforcement actions escalate.
- Check OIG LEIE, SAM, and state Medicaid exclusion lists monthly.
- Resolve matches within 24–48 hours to prevent terminations.
- Keep logs for audits and future reference.
Data Accuracy and System Alignment
Accurate enrollment data across PECOS, NPPES, and state applications reduces the risk of nationwide termination. Misaligned provider rosters or outdated credentials create enforcement triggers.
Billing workflows should pause claims for unclear provider status and verify updates quickly. Regular reconciliations, edit trails, and quarterly audits ensure all information matches federal and state records.
- Reconcile provider rosters with federal databases monthly.
- Alert staff to expired licenses, mismatched NPIs, or address conflicts.
- Apply coding and billing rules consistently to avoid errors.
Internal Audit and Monitoring
Ongoing internal audits help identify gaps in provider enrollment and billing compliance before CMS cross-program termination enforcement takes effect. Regular monitoring ensures any discrepancies are corrected promptly.
Audit teams should track provider status, billing activity, and credential updates continuously. Dashboards and reporting tools help visualize risks and maintain accountability across departments.
- Conduct quarterly audits of all provider enrollment records.
- Compare claims submissions against verified provider status.
- Document findings and corrective actions for future CMS inquiries.
Appealing a Cross-Program Enrollment Ban
Short guidance for providers facing nationwide termination. Explains what to do, how to rebuild enrollment, and what to expect during the process, all tied to CMS cross‑program termination enforcement.
Appeal Process
The appeal starts by identifying the program that issued the termination and submitting the required documentation to the correct authority. Prompt action is critical to prevent further complications under CMS cross-program termination enforcement.
- Identify the program and reason for termination.
- Gather compliance records, corrections, and supporting documentation.
- Submit appeal following state or federal instructions precisely.
Provide evidence of corrective actions taken, including exclusion checks, credential updates, or billing adjustments. Clear documentation can reduce review time and improve the likelihood of a favorable outcome.
- Include logs of exclusion screenings and data updates.
- Attach statements from credentialing or compliance staff.
- Provide updated licenses, NPIs, or corrected documents.
Re-Enrollment Strategy
After correcting the cause of termination, providers must submit a re-enrollment application to the relevant programs. Alignment with PECOS, NPPES, and state records ensures the new submission avoids previous errors.
- Verify all data matches federal and state records.
- Submit required forms and supporting documents.
- Confirm all staff and locations are cleared of exclusion or credential issues.
Coordinate with credentialing, billing, and compliance teams to prevent repetition of past mistakes. Conduct a short internal audit before submission to minimize the risk of rejection or further enforcement.
- Check provider rosters, claims, and documentation.
- Update internal policies per CMS program integrity guidance.
- Keep detailed records of communications during re-enrollment.
Timeline and Expectations
The appeal and re-enrollment process can take weeks to months, depending on program workload and documentation quality. Providers must plan cash flow and resources accordingly under CMS cross-program termination enforcement.
- Establish temporary billing holds or limited service plans.
- Maintain a timeline of submissions, responses, and follow-ups.
- Prepare for requests for additional information from reviewers.
Regular communication with all teams ensures deadlines are met, and tasks aren’t overlooked. Documentation of each step improves readiness for future compliance checks or audits.
- Schedule weekly status checks until closure.
- Store all correspondence and decision notices.
- Update internal tracking systems once enrollment is restored.
Conclusion
CMS cross-program termination enforcement in 2026 has transformed provider compliance into a nationwide responsibility. Even a minor error in one state can trigger automatic termination from Medicare, Medicaid, and CHIP, making vigilance across credentialing, billing, and exclusion checks essential.
Healthcare teams must implement proactive monitoring, accurate data management, and regular audits to protect practice operations and patient care. Timely appeals and strategic re-enrollment planning provide a structured path to recover from terminations and maintain continuity across all CMS programs.
FAQs
What is CMS cross-program termination enforcement in 2026?
CMS cross-program termination enforcement means a provider terminated in one program is automatically removed from Medicare, Medicaid, and CHIP nationwide.
What triggers a cross-program termination?
Common triggers include exclusion screening failures, credentialing errors, and coding or billing violations identified during CMS audits.
How often should exclusion screening be performed?
Exclusion screening should be done at hire and at least monthly, aligning with federal and state database updates.
Can providers appeal a cross-program termination?
Yes, providers can appeal by submitting documentation proving compliance corrections to the relevant state or CMS authority.
How can organizations prevent cross-program termination risks?
Maintain accurate enrollment data, perform regular audits, and ensure consistent coordination between credentialing and billing teams.





