Why are claims still denied even when coding and documentation are correct? In 2026, healthcare providers and billing teams process over 6.4 billion claims annually, yet more than 12% of these claims are denied on first submission. A common issue is incorrect or missing taxonomy codes. Even when CPT and ICD codes are accurate, a mismatch in taxonomy can lead to immediate rejection or delayed payment, resulting in rework and revenue gaps.
Many payers now need taxonomy codes on professional claims, and claims without these are increasingly being denied at the front end. Denial rates range between 13% and 15% across payer types, indicating that claim rejection is not an exception but a common problem. Each refused claim might cost $25 to $62 to reprocess, imposing extra pressure on billing teams and delaying collections.
This guide explains what a taxonomy code is and how it affects claims, NPI records, and payer processing. It also outlines where errors occur, how to verify taxonomy codes using the NPI registry, and how to correct mismatches. The goal is to help billing teams, coders, and providers reduce denials, improve claim accuracy, and maintain compliance with current payer requirements.
What Is a Taxonomy Code?
A taxonomy code is directly tied to provider classification in NPI records and payer systems. If the code does not match the enrolled specialty or is missing, claims may fail during front-end edits or be underpaid. Understanding this code is essential for Medical Billing Specialists, Coders, Credentialing Teams, and Revenue Cycle professionals working to reduce preventable denials.
This section explains what a taxonomy code is, how it functions in healthcare data systems, and why it affects billing accuracy and reimbursement outcomes. It focuses on definition and purpose, especially in relation to NPI registration, payer validation, and claim processing workflows.
Definition of a Taxonomy Code
A taxonomy code is a 10-character alphanumeric identifier used to classify healthcare providers by type, specialty, and classification. It is assigned through the National Uniform Claim Committee (NUCC) code set and used in the National Provider Identifier (NPI) system.
Key points:
- Identifies provider specialty and role
- Required during NPI enrollment in NPPES
- Used in electronic and paper claims
- Helps payers validate provider identity
Why Taxonomy Codes Exist
Taxonomy codes exist to standardize how healthcare providers are identified across billing, credentialing, and insurance systems. They ensure that every provider is classified under a consistent structure that payers and clearinghouses can verify.
Primary purposes include:
- Ensuring accurate provider identification in claims
- Supporting payer validation of specialty and services
- Reducing mismatches between NPI records and billing data
- Improving consistency in credentialing and enrollment processes
H2: Provider Taxonomy Code Structure and Levels
This section explains how taxonomy codes are structured, how classification levels work, and how examples translate into real-world billing use. It focuses on practical interpretation rather than theory; teams can apply it directly in NPI registration, claim submission, and payer verification workflows.
Three Levels of Taxonomy Codes
Taxonomy codes follow a structured classification system that defines provider identity in a standardized format used across NPPES, NUCC, and payer systems.
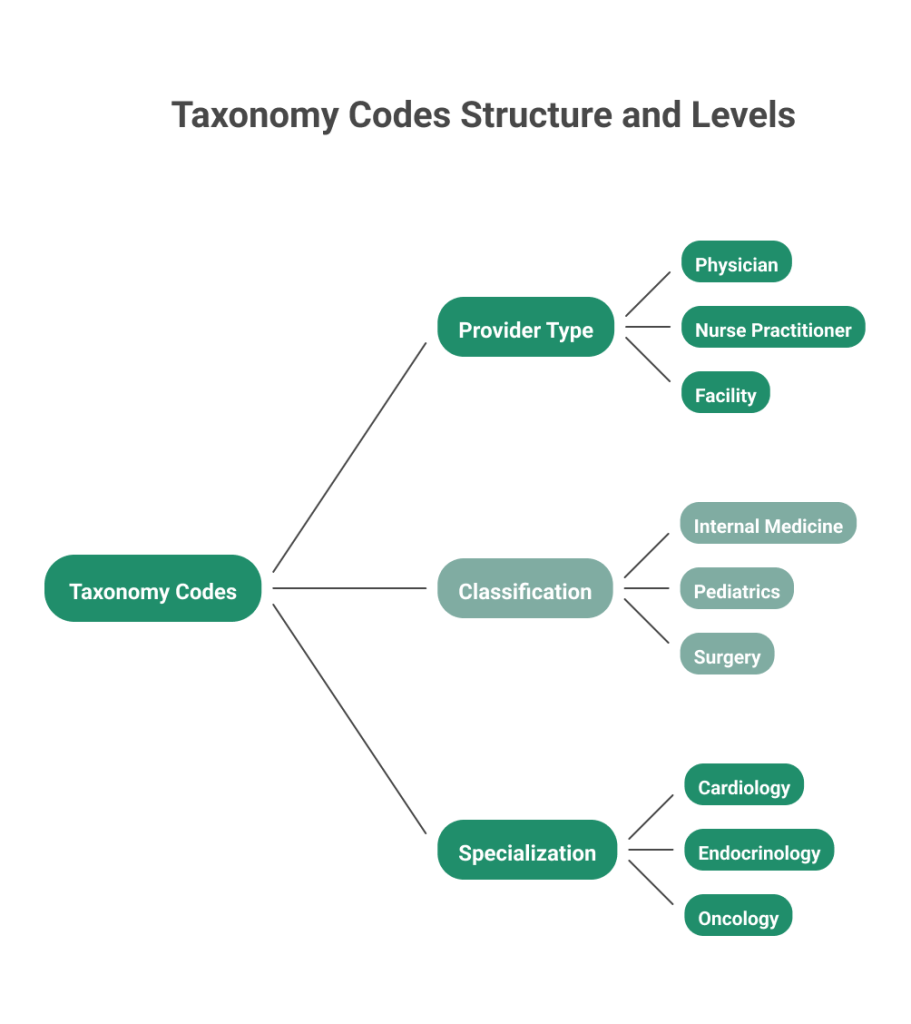
The structure is divided into three levels:
1. Provider Type
- Broad category of healthcare provider
- Example: Physician, Nurse Practitioner, Facility
- Used to define a general professional group
2. Classification
- Defines a medical field or discipline
- Example: Internal Medicine, Pediatrics, Surgery
- Helps narrow the provider category for billing accuracy
3. Specialization
- Defines a focused area of practice
- Example: Cardiology, Endocrinology, Oncology
- Used by payers for claim validation and reimbursement alignment
Example of a Taxonomy Code
A taxonomy code is structured to reflect provider classification and specialty in a standardized format used across NPI, NUCC, and payer systems. The breakdown below shows how each part of the code contributes to provider identification and billing accuracy.
| Component | Description | Example Value |
| Provider Type | Broad category of provider | 207 |
| Classification | Medical field or discipline | RC |
| Specialization | Specific area of practice | 0000X |
| Full Taxonomy Code | Complete 10-character identifier | 207RC0000X |
The Purpose of a Taxonomy Code in Medical Billing
Many claim rejections in 2026 are not caused by CPT or ICD errors, but by mismatched or missing taxonomy codes. With denial rates still above 12% across U.S. payers and front-end claim rejections increasing due to stricter validation rules, taxonomy accuracy has become a required step in clean claim submission.
This section explains how taxonomy codes function in medical billing workflows, especially in claims submission and payer processing. It focuses on operational use, not definitions, so billing teams can apply it directly in daily practice.
Role in Claims Submission
Taxonomy codes are used during claim submission to identify the provider’s specialty and validate billing data before processing begins.
Key functions in claims submission:
1. Required in electronic claims (837P) and CMS-1500 forms
2. Linked to provider NPI in billing systems
3. Helps clearinghouses verify provider classification
4. Ensures services match enrolled specialty
Role in Payer Processing
Taxonomy codes also play a direct role in how payers process, validate, and approve claims.
Key functions in payer processing:
1. Confirms provider specialty against payer enrollment records
2. Supports claim routing to correct review departments
3. Validates eligibility for billed services
4. Reduces the risk of underpayment or denial due to a mismatch
Taxonomy Code for NPI and NPPES
For Medical Billing Specialists, Credentialing Teams, and Revenue Cycle professionals, the NPI registry is the primary source of truth for provider classification. Any incorrect or outdated taxonomy entry in NPPES can affect claim acceptance, payer enrollment, and reimbursement outcomes.
This section explains how taxonomy codes function within NPI registration and how primary and secondary taxonomy selections impact billing accuracy and payer validation.
Role in NPI Registration
Taxonomy codes are required during the NPI registration process in the NPPES system. They define the provider’s specialty and are used by payers and clearinghouses to validate identity before claims are processed.
Key points:
- Taxonomy code must be selected when applying for an NPI
- It must match the provider’s actual specialty and credentials
- Providers must reference the NUCC taxonomy code set during selection
- Incorrect selection can lead to downstream claim rejections
Primary vs Secondary Taxonomy Code
Providers can assign more than one taxonomy code to a single NPI, but only one is marked as primary. This distinction plays a direct role in billing and payer validation.
Key differences:
Primary Taxonomy Code
- Represents the main area of practice
- Used most frequently in claim validation
- Often determines reimbursement routing
Secondary Taxonomy Code
- Represents additional specialties or services
- Used for secondary or limited billing scenarios
- Supports broader provider classification
Where Taxonomy Codes Are Used in Healthcare Systems
Taxonomy codes are not limited to registration or claim forms. They are used across multiple healthcare systems to validate provider identity, specialty, and billing eligibility. In 2026, payer systems and clearinghouses increasingly cross-check taxonomy data across platforms, contributing to stricter claim validation rules and higher front-end rejection rates when mismatches occur.
NPI Registry (NPPES)
The NPI Registry in NPPES is the official system, where taxonomy codes are stored and verified for each provider. It shows the provider’s primary and secondary taxonomy linked to their NPI record. This data is used as a reference point across billing and payer systems.
In 2026, many payers perform direct validation against NPPES before accepting claims. If the taxonomy code on a claim does not match the registry record, it can trigger a rejection. This makes the NPI Registry a critical source for ensuring billing accuracy and compliance.
Credentialing and Enrollment Systems
Credentialing and enrollment systems use taxonomy codes to confirm provider specialty during onboarding. These systems ensure that the provider’s classification matches payer requirements before approving network participation. Taxonomy accuracy is required for CAQH and payer applications.
If taxonomy data differs between credentialing records and NPI registration, delays or denials may occur. Payers rely on consistent taxonomy information to validate eligibility and contract status. For billing and credentialing teams, alignment across all systems is essential for uninterrupted claim processing.
Why Taxonomy Codes Cause Claim Denials
Payers use taxonomy codes to verify provider specialty before processing claims. If the taxonomy does not match enrollment or NPPES records, the claim is often stopped at the front end. This section explains the most common denial triggers and how they affect billing performance and reimbursement flow.
Common Denial Scenarios
Taxonomy-related denials usually occur when provider data does not match payer or NPI records. These issues are often detected during automated claim validation, leading to immediate rejection or return to the provider.
Common scenarios include:
1. Taxonomy code missing on claim submission
2. Primary taxonomy not matching billed service
3. Mismatch between NPI registry and payer enrollment records
4. Incorrect selection during NPI registration in NPPES
Impact on Revenue Cycle
Taxonomy errors directly affect revenue cycle performance by delaying claim acceptance and payment. Each rejected claim requires correction, resubmission, and additional administrative work, increasing operational cost for billing teams.
In 2026, claim rework costs range from $25 to $62 per denied claim, depending on payer and workflow complexity. These delays also slow down cash flow and increase days in accounts receivable (A/R). For Revenue Cycle teams, repeated taxonomy errors reduce overall collection efficiency and create avoidable revenue leakage.
How to Find a Taxonomy
Finding the appropriate taxonomy code is an essential step in NPI registration and claim setup. In 2026, payer systems will increasingly check taxonomy data in real time, although inaccurate selection will remain a source of claim denial and credentialing delays.
Using NUCC Code Set
The NUCC Code Set is the official source for all taxonomy codes used in healthcare billing and provider classification. It provides a structured list of provider types, classifications, and specialties used in NPI registration.
To find a taxonomy code using NUCC:
- Search by provider type or specialty
- Review classification and sub-specialty options
- Select the code that best matches the actual practice scope
- Verify before using it in NPI or claim submission
The NUCC list is updated periodically, and providers must ensure they are using the most current version. Incorrect selection from outdated lists can lead to claim mismatches and payer rejections.
Using NPI Registry
The NPI Registry (NPPES) allows users to search existing providers and view their assigned taxonomy codes. It is used for verification rather than selection during registration.
To use the NPI Registry:
- Search by provider name or NPI number
- Review the listed primary and secondary taxonomy codes
- Confirm alignment with provider specialty and billing records
Taxonomy Code for a Doctor and Other Providers
Understanding how taxonomy codes differ for doctors versus facilities is important for billing accuracy. Medical Billing Specialists, Coders, Credentialing Teams, and Revenue Cycle professionals must ensure the correct provider classification is used in NPI records and claims to avoid rejections and reimbursement delays.
Taxonomy Code for a Doctor
A taxonomy code for a doctor identifies the physician’s specialty within the healthcare system. It is used in NPI registration, credentialing, and claims processing to confirm provider identity and scope of practice.
Key points:
1. Based on a medical specialty such as internal medicine, cardiology, or pediatrics
2. Required during NPI enrollment in NPPES
3. Must match payer enrollment and credentialing records
4. Used in claims to validate billed services
Taxonomy Codes for Facilities and Organizations
Facilities and organizations also use taxonomy codes to define their service type and operational classification. These codes differ from individual provider taxonomy codes and are used for billing at the organizational level.
Key points:
1. Applied to hospitals, clinics, labs, and group practices
2. Represents facility type and service structure
3. Required for organizational NPI (Type 2 NPI)
4. Used for payer enrollment and claim routing
Conclusion
Taxonomy codes play a direct role in claim acceptance, NPI accuracy, and payer validation. In 2026, even small mismatches between taxonomy data and billing records continue to contribute to claim denials, delayed payments, and increased administrative rework across healthcare systems.
For Medical Billing, Coding, Credentialing, and Revenue Cycle teams, maintaining correct taxonomy alignment across NPPES, payer enrollment, and claims is a core requirement. Consistent accuracy reduces preventable denials, improves reimbursement flow, and supports compliance across all billing operations.
FAQs
What is a taxonomy code in medical billing?
A taxonomy code is a 10-character identifier used to classify healthcare providers by specialty and type. It is required in NPI registration and used in claims for provider identification and payer validation.
Why is a taxonomy code important for claims?
It helps payers confirm provider specialty before processing claims. Incorrect or missing taxonomy codes can lead to claim rejections, delayed payments, or reduced reimbursement.
Where can I find my taxonomy code?
You can find it using the NUCC Taxonomy Code Set or by searching the NPI Registry (NPPES). Both sources list valid provider classifications and specialties.
Can a provider have more than one taxonomy code?
Yes, a provider can have multiple taxonomy codes linked to a single NPI. However, only one is marked as the primary code, which represents the main area of practice.
Does a wrong taxonomy code affect NPI or credentialing?
Yes, incorrect taxonomy data can create mismatches in NPI records and credentialing systems. This may result in claim denials, enrollment delays, or payer rejections.





