Accurate credentialing documentation is critical for healthcare companies to check physician qualifications, ensure regulatory compliance, and facilitate payer registration. However, documentation errors remain a prevalent operational issue. Have you ever noticed why credentialing for some providers still takes up to 120 days in 2026, despite modern processes in place? Delays are frequently caused by incomplete, out-of-date, or improperly structured records, which distract providers from billing insurance and slow revenue output.
The financial impact is huge. Healthcare companies might lose approximately $7,500 per physician per day due to credentialing delays that restrict clinicians from seeing patients and submitting claims. Many hospitals also report quantifiable financial losses due to credentialing challenges, with some organizations losing more than $1 million per year because credentialing files are incomplete or verification processes are stalled.
Credentialing documentation management improves how provider records are collected, verified, stored, and monitored. Structured documentation workflows help credentialing specialists track license expirations, manage verification records, and maintain audit-ready files. This blog explains credentialing documentation requirements, digital workflow tools, compliance processes, and common documentation errors that affect provider onboarding and revenue cycle performance.
Credentialing Documentation Management
Credentialing documentation management ensures that all provider records, licenses, certifications, and compliance documents are accurate, complete, and readily accessible. Proper management reduces risk, improves operational efficiency, and supports regulatory compliance.
What Credentialing Documentation Includes
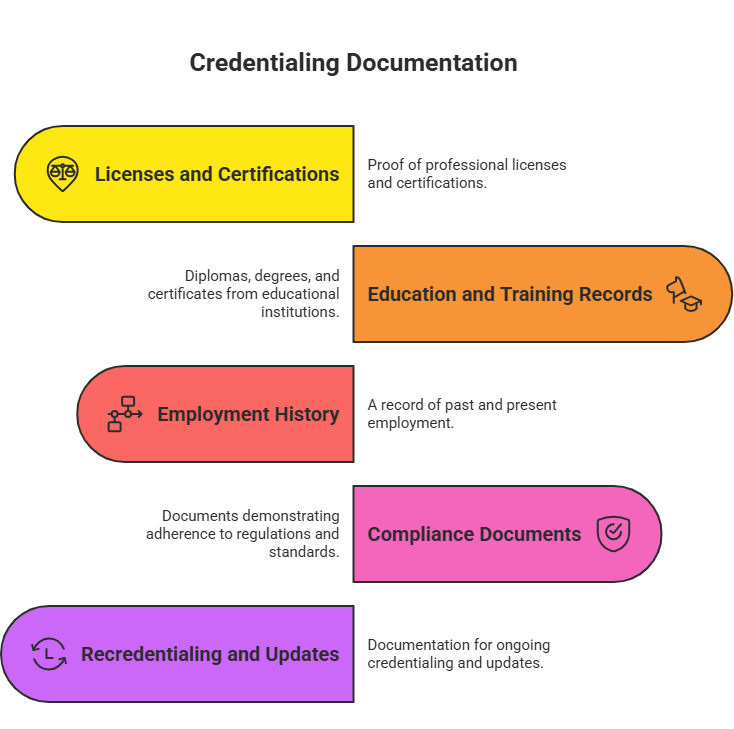
Credentialing documentation typically covers:
- Licenses and Certifications: State medical licenses, DEA registrations, board certifications, specialty permits.
- Education and Training Records: Medical school diplomas, residencies, fellowships, and continuing education certificates.
- Employment History: Previous affiliations, hospital privileges, gap verification.
- Compliance Documents: Background checks, malpractice insurance, immunization records, OSHA, and HIPAA training certificates.
- Recredentialing and Updates: Expiration dates, renewals, and amendments.
Why Documentation Management Matters for Healthcare Organizations
Healthcare organizations must maintain reliable credentialing records to:
1. Ensure Compliance: Meet regulatory standards such as HIPAA, The Joint Commission, and NCQA guidelines.
2. Reduce Risk: Avoid malpractice and credentialing errors that can lead to penalties.
3. Support Revenue Cycles: Credentialed providers can bill insurers without interruption, reducing lost revenue.
4. Improve Operational Efficiency: Centralized document tracking for credentialing enables faster verification and approvals.
5. Enhance Audit Readiness: Digital documentation workflows simplify audits and inspections, with real-time tracking and reporting.
Documentation Lifecycle in Credentialing
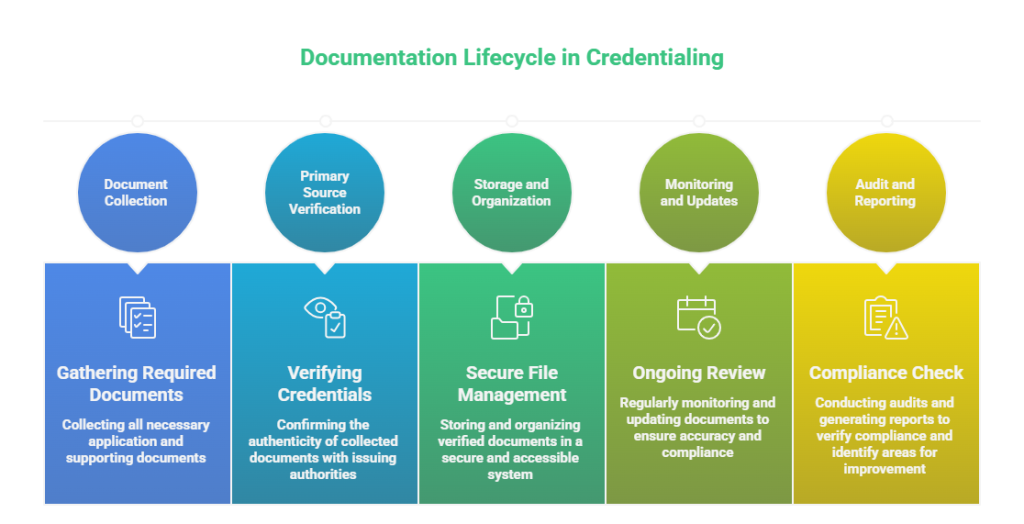
The credentialing documentation lifecycle includes the following stages:
1. Document Collection: Initial applications, verification requests, and provider-submitted documents.
2. Primary Source Verification: Confirming credentials with licensing boards, educational institutions, and previous employers.
3. Storage and Organization: Secure electronic or hybrid storage with controlled access.
4. Monitoring and Updates: Tracking expiration dates, renewals, and ongoing compliance requirements.
5. Audit and Reporting: Generating compliance-ready reports and dashboards for leadership review.
Digital Credentialing Workflow Tools
Digital credentialing workflow tools centralize and automate the management of provider documentation. They reduce errors, save staff time, and provide visibility into credentialing processes across healthcare organizations.
Credentialing Software for Providers
Credentialing software for providers helps healthcare teams collect, verify, and maintain credentialing documentation efficiently. Key capabilities include:
- Application Management: Collects provider applications digitally and flags missing information.
- Primary Source Verification: Confirms licenses, board certifications, and DEA registrations directly from authoritative sources.
- Automated Alerts: Notifies teams of upcoming expirations, recredentialing dates, and compliance deadlines.
Document Tracking for Credentialing
Document tracking for credentialing ensures all provider records are secure, organized, and accessible for audits or inspections. Effective tracking includes:
Centralized Storage: All documents are stored in a HIPAA-compliant system.
Access Controls: Staff permissions ensure sensitive data is protected.
Version Control: Tracks updates, re-submissions, and historical records.
Automated Reminders: Prompts teams for missing or expiring documents.
Integration With Revenue Cycle Systems
Integration of credentialing documentation management with revenue cycle systems improves billing accuracy and provider onboarding. Benefits include:
Faster Payer Enrollment: Verified provider credentials accelerate claims processing.
Reduced Denials: Accurate documentation prevents claim rejections due to credentialing issues.
Real-Time Updates: Credential status updates automatically feed into billing and payroll systems.
Data Consolidation: Combines credentialing and financial data for leadership reporting.
Credentialing Automation Best Practices
Credentialing automation best practices enhance accuracy, reduce manual tasks, and ensure compliance across all provider documentation. Automated systems help healthcare teams manage critical deadlines and maintain audit-ready records efficiently.
Standardized Credentialing Document Checklists
Standardized credentialing document checklists make the verification process easier and eliminate missing or incomplete files. Key points include:
Consistent Requirements: Lists all necessary documents for initial credentialing, recredentialing, and license renewals.
Error Prevention: Reduces mistakes caused by manual tracking and ad-hoc processes.
Digital Updates: Checklists automatically update based on state, payer, or organizational requirements.
Expiration Monitoring Systems
Expiration monitoring systems track license renewals, certifications, DEA registrations, and other critical credentials. Features include:
- Automated Alerts: Notify staff and providers of upcoming expirations to prevent lapses.
- Compliance Tracking: Ensures adherence to state, federal, and payer regulations.
- Reporting Capabilities: Provides real-time visibility into credential status and risk areas.
Centralized Credentialing Document Storage
Centralized document storage consolidates all credentialing records in a secure, accessible platform. Advantages include:
- HIPAA-Compliant Storage: Protects sensitive provider data with encrypted cloud or on-premises systems.
- Single Access Point: Teams can quickly locate and share documents for audits or payer submissions.
- Historical Tracking: Maintains version histories, updates, and previous submissions for transparency.
Compliance Documentation Workflow
The compliance documentation process ensures that all credentialing documents meet regulatory requirements while being available for audits. Streamlined workflows decrease errors, increase transparency, and help organizations meet compliance requirements.
Regulatory Requirements for Credentialing Documentation
Healthcare organizations must follow federal, state, and payer-specific regulations for credentialing documentation. Key requirements include:
- Licensure Verification: State medical boards, DEA registration, and controlled substance licenses.
- Certification Documentation: Board certifications, training completions, and continuing education.
- Policy Adherence: Standardized forms, retention schedules, and secure access controls.
Audit Preparation and Documentation Reviews
Regular audits and reviews keep credentialing documentation accurate and inspection-ready. Practices include:
- Scheduled Reviews: Quarterly or semiannual checks to confirm document validity.
- Checklist Verification: Ensures all required elements are present and current.
- Audit-Ready Reports: Generate organized reports for payers, regulators, or accreditation bodies.
Risk Reduction Through Documentation Control
Controlled documentation limits exposure to compliance and financial risks. Strategies include:
- Access Management: Define user permissions to prevent unauthorized edits or downloads.
- Version Tracking: Maintain historical versions of credentialing documents.
- Error Mitigation: Automated alerts flag missing, expired, or incorrect records.
Common Credentialing Documentation Errors
Identifying frequent documentation errors allows healthcare organizations to prevent delays and compliance issues. Correcting these errors early supports accurate credentialing and smooth revenue cycles.
Missing Provider Documents
Incomplete documentation is a leading cause of credentialing delays. Commonly missing items include:
- Medical licenses and DEA registrations
- Board certifications and continuing education records
- Hospital privileges and work history verification
Expired Credentials
Expired credentials create compliance risks and may halt provider onboarding. Key areas to monitor include:
- State licenses and DEA registrations
- Board certifications and specialty training
- Malpractice insurance coverage
Inconsistent Provider Data
Discrepancies in provider information cause verification failures and audit findings. Typical inconsistencies involve:
- Name variations across licenses, insurance, and payers
- Incorrect dates of licensure or training
- Mismatched specialty or practice details
Conclusion
Effective credentialing documentation management is essential for healthcare organizations to maintain compliance, reduce risk, and support uninterrupted revenue cycles. Implementing digital workflow tools, automation, and centralized storage ensures accurate, audit-ready records while minimizing errors.
By standardizing processes, monitoring expirations, and controlling documentation, healthcare teams can improve provider onboarding speed, prevent credentialing delays, and strengthen operational efficiency. Continuous review and proper management keep organizations prepared for audits and regulatory updates in 2026.
FAQs
What is credentialing documentation management?
Credentialing documentation management organizes, verifies, and stores provider credentials to ensure compliance and streamline onboarding. It supports audit readiness and reduces operational errors.
Why are digital credentialing workflow tools important?
Digital tools automate document collection, verification, and alerts, improving efficiency and reducing errors in credentialing processes. They provide visibility into provider records and deadlines.
What common errors occur in credentialing documentation?
Missing documents, expired credentials, and inconsistent provider data are frequent issues that delay onboarding and create compliance risks. Early detection prevents financial and operational setbacks.
How does automation improve credentialing workflows?
Automation tracks expirations, updates checklists, and generates reports, reducing manual tasks and maintaining audit-ready records. It speeds verification and supports revenue cycle continuity.
How can a compliance documentation workflow reduce risks?
Structured compliance workflows ensure documents meet federal, state, and payer regulations, prevent unauthorized access, and maintain accurate records for audits and regulatory inspections.





