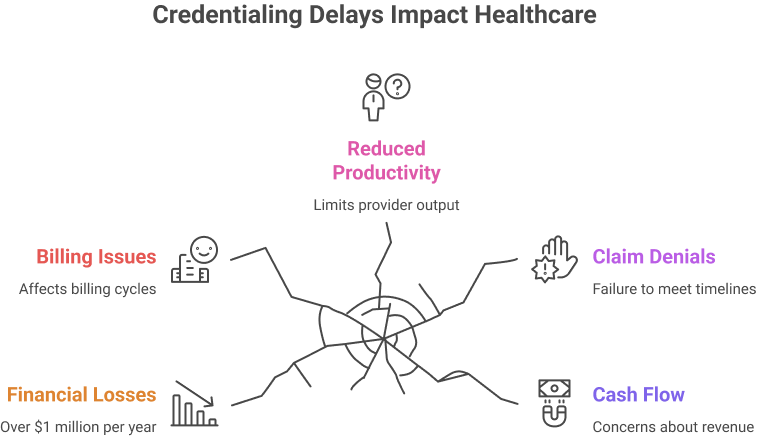
Credentialing delays provide major operational and financial challenges for healthcare providers, credentialing specialists, and billing teams. In 2026, over half of hospitals and provider groups estimate significant financial losses caused by credentialing issues, with several reporting losses of more than $1 million per year due to delayed enrollments and claim procedures. These delays affect billing cycles and limit provider productivity.
Credentialing and re-credentialing processes can take 90-120 days or longer, depending on payer type, records, and regulatory requirements. Failure to satisfy paperwork or follow-up timelines can result in claim denials, cash-flow concerns, and decreased patient access. Credentialing errors and missing information are key sources of these delays, which contribute to longer processing times and increased workload strain.
This guide describes medical re-credentialing, its importance for revenue cycle and compliance, and how to avoid typical errors. It outlines clear timelines, standards, and best practices that credentialing and revenue cycle personnel may use to prevent delays, maintain reimbursement, and keep providers in the network.
What is Medical Re-Credentialing?
Medical re-credentialing is a critical compliance process for healthcare providers, ensuring their qualifications, licensure, and certifications remain current. In 2026, delayed re-credentialing accounts for up to 15% of initial claim denials in U.S. practices, affecting significant operational and financial risk.
This section explains the purpose of medical re-credentialing and how it differs from initial credentialing, giving healthcare teams a clear roadmap to reduce errors and maintain in-network status.
Definition and Purpose
Medical re-credentialing is the periodic verification of a provider’s credentials, licenses, and certifications to maintain eligibility with insurance payers and regulatory bodies. This process protects patients, ensures compliance, and supports uninterrupted revenue cycles.
Key elements include:
- Verification of state licensure and DEA registration
- Review of board certifications and professional qualifications
- Evaluation of malpractice insurance coverage
- Assessment of work history and hospital privileges
- Screening for sanctions, exclusions, or disciplinary actions
Re-Credentialing vs Credentialing
Re-credentialing differs from initial credentialing in scope and timing:
Credentialing: Verifies provider eligibility before joining a payer network. This usually happens only once after you’re hired.
Re-credentialing: Periodic verification to ensure credentials remain valid, generally every 2–3 years. Some states, such as Illinois, require 3-year intervals.

Medical Re-Credentialing Timeline
Medical re-credentialing follows defined cycles that vary by provider type and payer requirements. Understanding timelines helps healthcare organizations prevent delays, avoid claim denials, and maintain compliance in 2026, when initial claim denials related to expired credentials reached 12% nationwide.
This section provides a clear overview of typical re-credentialing timelines and strategies to optimize the process for faster approvals and continuous payer participation.
Typical Timelines by Provider Type
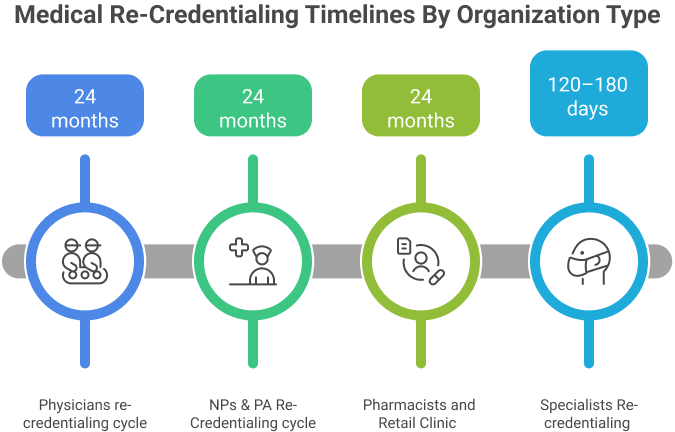
Re-credentialing timelines differ based on provider role and payer rules:
- Physicians: Every 24 months; some states allow 36 months. Average processing time: 90–150 days.
- Nurse Practitioners & Physician Assistants: Typically every 24 months. Processing time: 60–120 days.
- Pharmacists and Retail Clinic Providers: Usually every 24 months; 60–90 days for verification.
- Specialists (Behavioral Health, Anesthesiology, Surgery): May require additional documentation; 120–180 days average.
Timeline Optimization Strategies
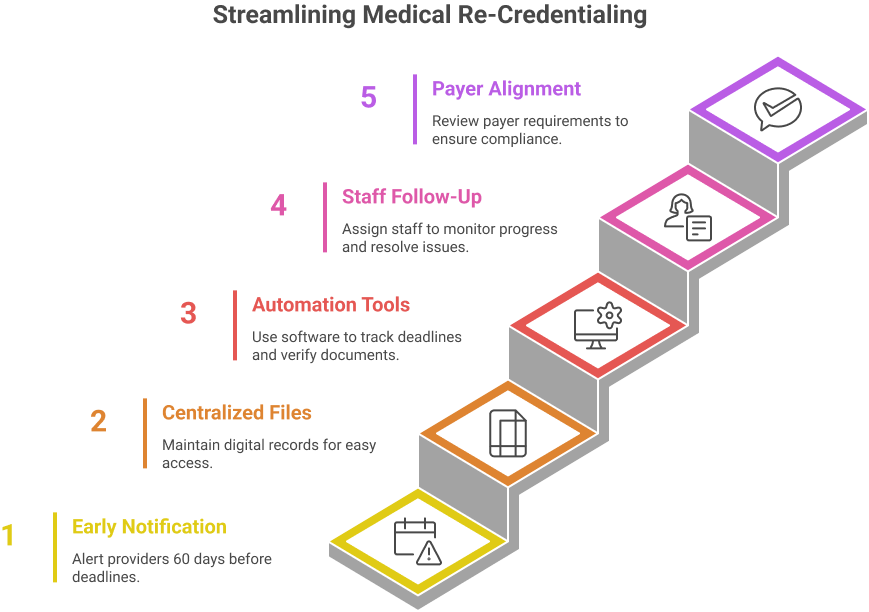
Healthcare organizations can reduce re-credentialing delays by implementing structured strategies:
1. Early Notification: Alert providers at least 60 days before re-credentialing deadlines.
2. Centralized Credentialing Files: Maintain digital files for licenses, DEA registration, board certifications, and malpractice coverage.
3. Automation Tools: Use credentialing software to track deadlines, send reminders, and verify primary source documentation.
4. Dedicated Staff Follow-Up: Assign a staff member to monitor the progress of applications and resolve discrepancies quickly.
5. Payer Rule Alignment: Review each payer’s re-credentialing requirements to avoid compliance gaps.
Re-Credentialing Requirements for Providers
Medical re-credentialing requires specific documentation and verification to maintain provider eligibility. Missing or incomplete information can delay approval, affect reimbursements, and risk compliance violations.
This section outlines the core and additional requirements providers must submit during the re-credentialing process to meet payer and regulatory standards.
Core Documentation Required
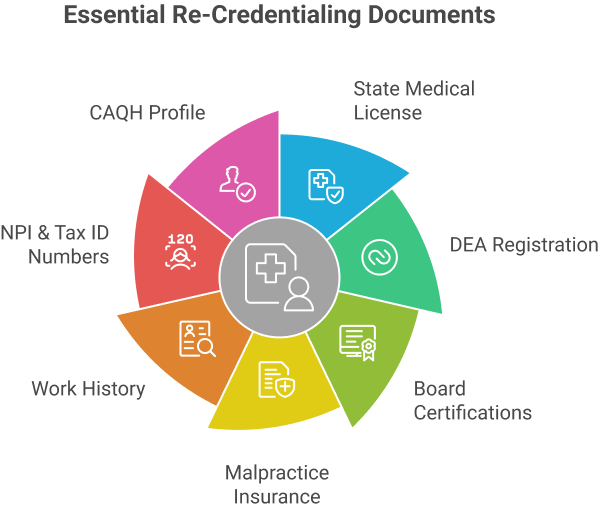
Providers must submit essential documents to maintain network participation and avoid claim disruptions:
- State Medical License: Current and in good standing with the licensing board.
- DEA Registration (if applicable): Active registration for providers prescribing controlled substances.
- Board Certifications: Proof of current board certifications relevant to specialty.
- Malpractice Insurance: Updated coverage and claims history.
- Work History and Professional References: Complete employment history with verifiable references.
- NPI & Tax Identification Numbers: Ensure these identifiers are current and accurate.
- CAQH Profile (if used): Updated and fully verified provider profile.
Optional or Additional Requirements
Some payers may require supplementary documents to verify compliance and enhance patient safety:
- Continuing Education Records: Proof of CME/CEU completion within the past cycle.
- Affiliation or Hospital Privileges: Verification of current clinical affiliations.
- State-specific Certifications or Licenses: Additional state licenses, permits, or specialty certifications.
- Background Checks: Criminal history verification in states or payers requiring extra screening.
- Compliance Training Certificates: HIPAA, OSHA, or other mandatory compliance certifications.
Common Re-Credentialing Mistakes to Avoid
Errors in medical re-credentialing can cause delays, interruptions in billing, and compliance penalties. Understanding typical risks and how to avoid them is crucial for both clinicians and credentialing personnel.
This section identifies frequent mistakes in the provider re-credentialing process and practical steps to mitigate them effectively.
Frequent Errors
Incomplete Applications: Missing licenses, certifications, or insurance documentation can stall the approval process.
Expired Credentials: Submitting outdated state licenses, DEA registration, or board certifications leads to delays.
Failure to Follow Up: Neglecting to track progress with payers can prolong credentialing by weeks or months.
Misunderstanding Enrollment vs Credentialing: Confusing the two processes may result in denied claims or missed billing opportunities.
Ignoring Re-Credentialing Deadlines: Late submissions disrupt provider network participation and can impact reimbursements.
Mitigation Tips
1. Use a Centralized Credentialing Tracker to keep current data and track due dates for each provider.
2. Verify All Documents Before Submission: Cross-check licenses, certifications, insurance, and NPI numbers for accuracy.
3. Automate Reminders: Credentialing software can alert staff and providers about upcoming expirations.
4. Educate Staff on Process Differences: Clarify the distinction between credentialing and enrollment to avoid errors.
5. Start Early: Begin re-credentialing 90–180 days before the current credential expires to allow time for corrections.
Conclusion
Medical re-credentialing is a critical process that protects provider eligibility, maintains compliance, and ensures uninterrupted revenue cycles. Timely and accurate completion prevents claim denials, cash-flow disruptions, and network participation issues.
Implementing structured workflows, centralized documentation, and automated reminders allows healthcare organizations to reduce delays and maintain efficient re-credentialing cycles. Proactive management strengthens provider credibility, supports compliance, and safeguards operational and financial performance.
FAQs
What is medical re-credentialing?
Medical re-credentialing is the periodic verification of a provider’s licenses, certifications, and qualifications to maintain eligibility with payers and ensure compliance.
How often does re-credentialing occur?
Most providers undergo re-credentialing every 24 to 36 months, depending on payer rules and state-specific regulations.
What documents are required for re-credentialing?
Core documents include state licenses, DEA registration, board certifications, malpractice insurance, work history, and updated NPI/CAQH profiles.
What are common re-credentialing mistakes to avoid?
Frequent errors include missing documents, expired credentials, delayed submissions, and confusing credentialing with enrollment.
How can organizations streamline the re-credentialing process?
Use centralized credentialing trackers, automated reminders, early notifications, and dedicated staff to verify and follow up on all documentation.





