Medicare credentialing will continue to be an important challenge for provider enrollment and revenue cycle operations in 2026. The entire Medicare population continues to grow, with approximately 68.9 million people enrolled in Medicare as of 2025 and over 62.8 million covered under Parts A and B, a statistic that continues to rise as more Americans become eligible each year. To avoid denials and revenue loss, physicians, medical billers, and practice administrators must ensure proper Part B enrollment as the pool grows.
Enrollment timing and payer compliance difficulties are also influencing industry expectations. Many providers’ Medicare credentialing and payer enrollment durations have increased, with provider enrollment timeframes averaging 90 to 180 days across payers as data validation and documentation standards become increasingly severe. When applications are incomplete or incorrect, they have an immediate impact on billing operations and cash flow, causing over 40% of all enrollment delays.
This guide explains Medicare credentialing from a compliance and billing standpoint. It outlines the process, timelines, and common mistakes while highlighting where providers gain stability and where errors create problems. The goal is to help healthcare providers, credentialing specialists, and billing teams complete Medicare credentialing accurately and avoid disruptions tied to Part B enrollment.
What Is Medicare Credentialing
Medicare Credentialing ensures that healthcare providers meet CMS standards to participate in Medicare Part B. It verifies credentials, licensure, and compliance before billing federal programs.
This section explains the difference between credentialing and enrollment and identifies which providers must complete Medicare Part B enrollment to legally bill Medicare.
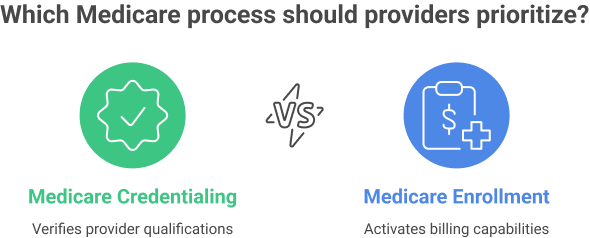
Medicare Credentialing vs. Medicare Enrollment
Medicare credentialing confirms that a provider’s education, licensure, training, and professional background meet CMS requirements. Enrollment, on the other hand, is the official process of registering with Medicare to receive a provider number and bill for services.
Key points:
- Credentialing focuses on verification and compliance.
- Enrollment activates the provider’s ability to bill Medicare Part B.
- Both steps are mandatory to prevent claim denials or delayed payments.
Providers Required to Complete Medicare Part B Enrollment
Not all healthcare providers automatically qualify. Providers required to complete Medicare Part B enrollment include:
- Physicians and surgeons (MD, DO)
- Nurse practitioners, physician assistants, and clinical nurse specialists
- Physical therapists, occupational therapists, and speech-language pathologists
- Licensed professional counselors and mental health practitioners billing Medicare.
- Group practices or clinics intending to bill Part B under a shared NPI
Medicare Credentialing
Medicare Credentialing verifies that healthcare providers meet CMS standards to participate in Medicare Part B. This process ensures compliance, protects billing rights, and confirms provider qualifications.
In this section, we explain the role of CMS in credentialing and how proper credentialing affects claims, payments, and provider credibility.
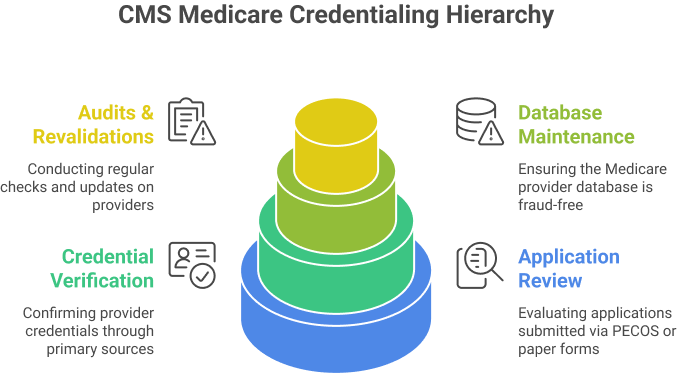
Role of CMS in Medicare Credentialing
The Centers for Medicare & Medicaid Services (CMS) oversees all provider enrollment and credentialing activities. CMS ensures that providers meet federal standards for licensure, education, training, and background checks.
Key responsibilities include:
- Reviewing applications submitted via PECOS or paper forms.
- Verifying credentials through primary source checks.
- Maintaining the Medicare provider database to prevent fraud or improper billing.
- Conducting regular audits and revalidations of providers.
Impact of Medicare Credentialing on Claims and Payments
Accurate Medicare credentialing directly affects claims submission and reimbursement. Providers with incomplete or incorrect enrollment can face claim denials, delayed payments, or compliance penalties.
Key points:
- Credentialed providers receive a unique Medicare provider number required for billing.
- Proper enrollment ensures timely payment from Medicare for Part B services.
- Credentialing errors can result in claim rejections, audits, or loss of eligibility.
- Maintaining up-to-date information in PECOS prevents administrative errors and reduces the risk of penalties.
Medicare Credentialing Process for Part B Providers
Medicare Credentialing ensures that Part B providers meet CMS requirements to deliver services to Medicare beneficiaries. This process validates credentials, protects claims reimbursement, and establishes compliance with federal regulations.
In this section, we break down the Part B credentialing process into actionable steps. Providers can follow these steps to complete enrollment efficiently while avoiding common errors that delay billing and payments.
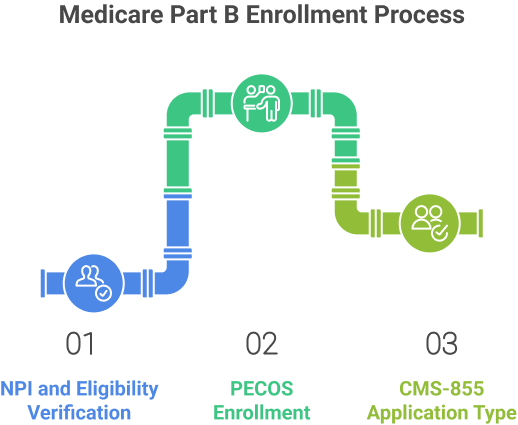
Step 1: NPI and Eligibility Verification
Before starting Medicare Part B enrollment, providers must confirm eligibility and obtain a National Provider Identifier (NPI).
Key points:
- Providers must hold a valid state license and demonstrate professional liability coverage.
- NPI verification confirms the provider type, specialty, and practice location.
- Eligibility checks prevent future claim denials and ensure compliance with CMS requirements.
Step 2: PECOS Enrollment for Doctors
PECOS is the online Medicare enrollment system that simplifies the Part B credentialing process.
- Submit your enrollment application electronically for faster processing.
- Upload all required documentation, including licensure, NPI, and liability insurance.
- PECOS tracks application status and allows electronic signatures to complete enrollment.
- Providers who submit via PECOS typically experience fewer errors compared to paper applications.
Step 3: CMS-855 Application Type
The CMS-855 forms define the enrollment category and ensure accurate credentialing.
- CMS-855I: Used for physicians and non-physician practitioners.
- CMS-855O: For ordering and certifying providers.
- CMS-588: EFT Authorization for direct payments.
- Forms must be signed, complete, and submitted to the appropriate Medicare Administrative Contractor (MAC).
- Selecting the correct form prevents processing delays and claim rejections.
Medicare Part B Enrollment for Providers
Medicare Part B enrollment is essential for providers to bill for outpatient services. This process ensures compliance with CMS rules and grants access to Medicare reimbursements.
Providers must meet specific requirements and submit proper documentation to start serving Medicare beneficiaries under Part B. Understanding effective dates and billing privileges prevents payment delays and claim denials.
Enrollment Requirements by Provider Type
- Physicians and Non-Physician Practitioners: Must submit CMS-855I with a valid state license, NPI, and professional liability coverage.
- Group Practices and Clinics: Use CMS-855B, including group NPI, ownership details, and practice locations.
- Ordering, Referring, or Certifying Providers: Submit CMS-855O to authorize services and prescriptions under Medicare Part B.
- Specialty Providers (e.g., Pharmacies, DME Suppliers): Submit applicable CMS forms and supporting documentation per CMS guidelines.
Effective Dates and Billing Privileges
- Enrollment is effective the first day of the month after CMS approval, unless a retroactive effective date applies.
- Once approved, providers can submit claims for Medicare Part B-covered services.
- Timely submission of applications and documents ensures billing privileges start without gaps, reducing revenue interruptions.
- PECOS enrollment can speed up processing compared to paper applications, making providers eligible sooner.
Medicare Provider Enrollment Timeline
Understanding the Medicare provider enrollment timeline helps healthcare practices plan for claims submission and revenue flow. Delays in enrollment can lead to missed reimbursements or denied claims.
The timeline varies depending on the provider type, application method, and CMS processing times. Providers should track progress to ensure billing privileges start promptly.
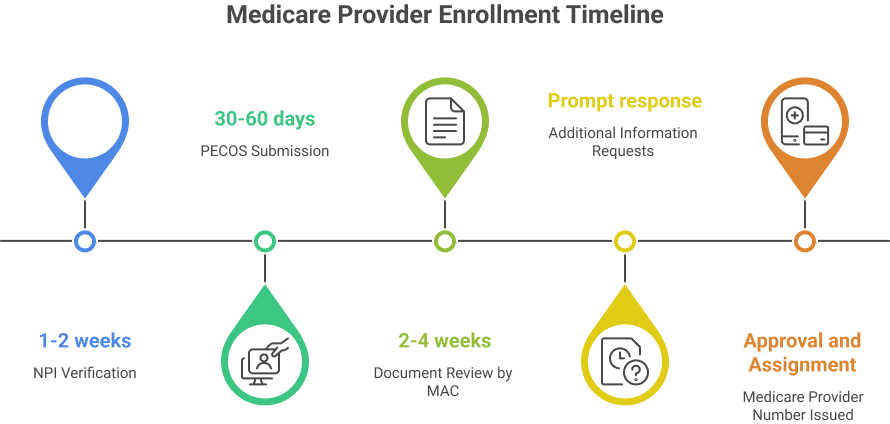
Typical Enrollment Steps and Duration
1. NPI Verification – Confirm your National Provider Identifier (NPI). This usually takes 1–2 weeks if applied through NPPES.
2. PECOS Submission – Online application processing through PECOS typically takes 30–60 days, faster than paper submissions.
3. Document Review by MAC – CMS or your Medicare Administrative Contractor (MAC) reviews applications and supporting documentation, often taking 2–4 weeks.
4. Additional Information Requests – If MAC requests clarifications, respond promptly. Delays here can extend the timeline.
5. Approval and Assignment of Medicare Provider Number – Once approved, your Medicare provider number is issued, activating billing privileges.
Key Points to Maintain Timeline
Here are the key points to maintain the timeline:
- Start applications early to avoid gaps in coverage.
- Ensure all documents are accurate and complete to prevent rejections.
- Track your PECOS application regularly and respond promptly to MAC requests.
- Typical total duration from initial submission to full enrollment is 6–12 weeks, depending on provider type and completeness of the application.
Common Medicare Credentialing Mistakes
Even experienced healthcare providers and credentialing specialists can face delays or denials if errors occur during Medicare credentialing. Knowing common mistakes helps prevent lost revenue and unnecessary complications.
Errors in PECOS Enrollment
Incomplete Applications: Missing required documents, such as NPI verification, state licenses, or liability insurance proof, can delay approval.
Incorrect Data Entry: Errors in provider information, Tax ID, or credentials can trigger rejections. Always double-check every field before submission.
Delayed Responses to MAC Requests: Failure to respond promptly to Medicare Administrative Contractor (MAC) inquiries can extend processing times by weeks.
Practice Location and Reassignment Issues
Incorrect Practice Addresses: Ensure practice locations are accurately listed in PECOS. Errors affect claims routing and payment processing.
Reassignment of Benefits Mistakes: When billing through a group or clinic, mismanaged reassignment forms can lead to denied claims or delayed reimbursements.
Failure to Update Changes: Changes in ownership, location, or provider status must be reported within 30–90 days to maintain billing privileges.
Conclusion
Accurate Medicare credentialing and Part B enrollment are essential for maintaining compliance, securing timely payments, and supporting practice revenue. Providers, credentialing specialists, and billing teams who complete the process correctly reduce claim denials and administrative delays.
By following the outlined steps, adhering to PECOS requirements, and avoiding common errors, healthcare practices can streamline enrollment, maintain uninterrupted billing privileges, and confidently serve Medicare beneficiaries. Effective credentialing safeguards both compliance and financial operations.
FAQs
What is Medicare credentialing?
Medicare credentialing verifies a provider’s licensure, credentials, and compliance with CMS standards before billing Part B services.
Who must complete Medicare Part B enrollment?
Physicians, non-physician practitioners, therapists, and group practices intending to bill Medicare Part B must complete enrollment.
How long does the Medicare credentialing process take?
Enrollment typically takes 6–12 weeks, depending on provider type, document completeness, and PECOS or MAC processing times.
What are common Medicare credentialing mistakes?
Errors include incomplete PECOS applications, incorrect provider details, delayed responses to MAC requests, and mismanaged reassignment forms.
How can PECOS enrollment speed up Part B credentialing?
Submitting applications electronically via PECOS reduces errors, allows document uploads, tracks status, and enables faster processing than paper forms.





