Accurate provider directory data remains a persistent problem across healthcare systems. Why do patients still receive out-of-network bills even when they confirm their provider is in-network? Studies and field reports indicate that provider directories can still be 40–80% inaccurate in 2026, with errors in location, specialty, and network status common across major payer lists. These inaccuracies lead to claim denials, compliance risk, and poor patient experience for both payers and providers.
The No Surprises Act provider directory compliance requirements aim to correct these failures and protect patients from unexpected out-of-network bills. Under the Act and CMS guidance, health plans and providers must verify directory data at least every 90 days and update it promptly when changes occur.
Non-compliance carries real financial risk. Civil penalties and corrective action plans may apply, with enforcement tied to data accuracy, timely updates, and audit readiness. These rules place pressure on billing teams, credentialing staff, and compliance officers to maintain consistent, verified provider data across all systems. This guide explains both the risks and the operational benefits of compliance. It shows how accurate provider data reduces claim denials, prevents penalties, and supports audit readiness.
Provider Directory Accuracy & The No Surprises Act
This section explains federal requirements for provider directory accuracy. It outlines how compliance impacts billing, credentialing, and audit risk.
What the No Surprises Act Requires for Provider Directories
The No Surprises Act provider directory compliance framework sets strict rules for health plans and providers. It aligns with the CMS ghost network regulation, which targets outdated and incorrect directory listings. The goal is to ensure patients can rely on accurate in-network information.
The Consolidated Appropriations Act (CAA) strengthens enforcement. It requires plans to maintain correct provider data and reduce misinformation across directories.
Key compliance requirements include:
90-day verification rule: Health plans must confirm directory data at least every 90 days.
Timely updates: Providers must report changes in address, specialty, and network status quickly.
Health plan provider data accuracy: Systems must reflect current, verified information.
Error correction timelines: Incorrect listings must be corrected once identified.
Audit readiness: Records must support compliance during regulatory review.
Why Provider Directory Accuracy Matters
Provider directory accuracy directly impacts billing, compliance, and patient trust. Errors lead to claim denials, payment delays, and increased administrative workload for billing teams. They also create disputes, refunds, and operational inefficiencies across the revenue cycle.
Inaccurate data increases risk under the No Surprises Act provider directory compliance and CMS ghost-network regulations. It can trigger audits, financial penalties, and reduced transparency for patients. Accurate directories support faster claims processing, better coordination, and stronger compliance with federal mandates.
CMS Ghost Network Regulation and Real-World Risk
The CMS ghost network regulation addresses inaccurate provider listings that show providers as in-network when they are not available or active. This creates real risk for claims, patient access, and No Surprises Act provider directory compliance.
Errors can lead to claim denials, billing disputes, and regulatory action. Poor health plan provider data accuracy increases exposure to audits, penalties, and loss of patient trust.
What Is a Ghost Network
The No Surprises Act provider directory compliance rules address a major issue known as the CMS ghost network regulation. A ghost network occurs when a provider directory lists clinicians who are not actually available, not in-network, or no longer practicing at that location.
Under the Consolidated Appropriations Act (CAA), payers must maintain accurate provider data. The 90-day verification rule requires regular confirmation of listings to prevent outdated or misleading entries.
Ghost networks arise from:
- Outdated provider records have not been removed from directories
- Failure to update practice location or network participation
- Delays in credentialing and enrollment updates
- Ghost networks often stem from administrative backlogs; utilizing professional Physician Enrollment Services ensures your provider data is updated with payers in real-time to prevent these discrepancies.
- Poor coordination between payer systems and provider data
Impact of Ghost Networks on Providers and Patients
Ghost networks affect both financial operations and patient care. The impact extends across billing, compliance, and access to care.
For patients:
- They may choose an “in-network” provider who is actually out-of-network
- They face unexpected medical bills under the No Surprises Act
- They experience delays in receiving care due to incorrect listings
For providers and billing teams:
- Claim rejections increase due to a mismatched network status
- Appeals and corrections consume additional resources
- Payment delays occur due to payer disputes
- Payer disputes regarding network participation can often be resolved or prevented by ensuring your Healthcare Contracting Services are correctly aligned with the information listed in public directories.
- Administrative burden rises across billing and credentialing teams
For payers and compliance teams:
- Violations of the No Surprises Act provider directory compliance requirements
- Risk of enforcement under CMS ghost network regulation
- Exposure to audits and civil monetary penalties (CMP)
- Loss of trust in the health plan provider’s data accuracy systems
90-Day Verification Rule and 2-Day Update Requirement
The 90-day verification rule requires health plans to confirm provider directory data at least every 90 days. This supports the No Surprises Act provider directory compliance and improves the provider’s correct data for the health plan. Regular checks reduce outdated or incorrect listings.
The 2-day update requirement mandates that any provider changes be updated within two business days. This includes changes in location, network status, or contact details. Timely updates reduce risk under CMS ghost network regulation and help avoid civil monetary penalties (CMP).
For virtual care providers, maintaining directory compliance is critical; specialized Telehealth Credentialing Services can help manage these rapid updates for remote network status.
90-Day Verification Rule Explained
The No Surprises Act provider directory compliance framework requires health plans to verify provider data every 90 days. This rule aligns with health plan provider data accuracy standards set under federal guidance and the Consolidated Appropriations Act (CAA).
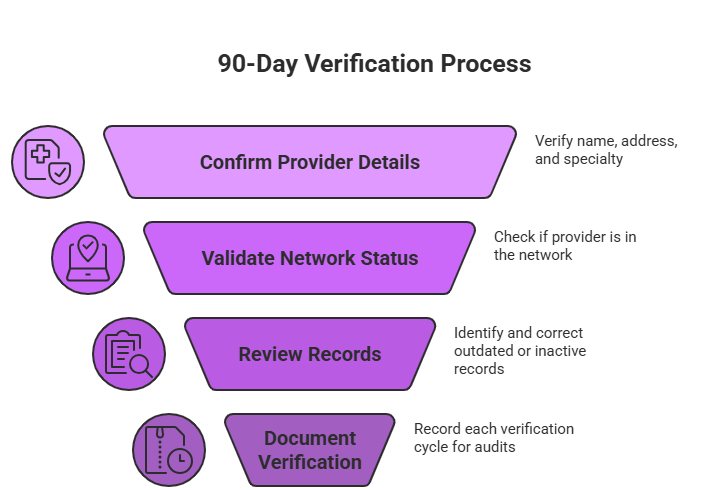
The 90-day verification rule requires plans to:
- Confirm provider name, address, and specialty
- Validate network participation status
- Review and correct outdated or inactive records
- Document each verification cycle for audit purposes
2-Day Update Requirement
The No Surprises Act provider directory compliance rules also include a 2-day update requirement. This rule applies when providers report changes in their data.
Once a provider notifies a change, the plan must update the directory within 2 business days. This includes:
- Changes in practice location
- Network participation updates
- Specialty or service updates
- Termination or addition of providers
Civil Monetary Penalties (CMP) and Inaccurate Directory Fines
This section explains financial penalties linked to directory non-compliance. It outlines how enforcement actions affect providers, plans, and revenue cycle operations.
CMP Structure and Financial Exposure
The No Surprises Act provider directory compliance rules establish clear financial penalties for inaccurate data. These penalties fall under civil monetary penalties (CMP) and are enforced alongside the CMS ghost network regulation. Financial exposure increases when errors are repeated or left uncorrected over time.
CMP exposure depends on multiple factors. These include the number of affected patients, duration of inaccurate listings, and failure to meet the health plan provider data accuracy standards. The Consolidated Appropriations Act (CAA) strengthens enforcement and expands penalty authority for the regulators.
Fines may be issued per violation and can accumulate quickly. Repeated issues raise total liability and trigger additional review. This leads to inaccurate directory fines that impact both financial performance and compliance standing.
Audit Process and Enforcement Timeline
The No Surprises Act provider directory compliance enforcement process starts with a formal audit of provider directory data. Regulators review listings, compare them with reported information, and identify gaps. These reviews focus on accuracy, updates, and compliance with federal rules.
If errors are found, regulators issue a correction notice. Health plans must respond within a defined timeframe. Failure to correct issues can lead to civil monetary penalties (CMP) and further investigation under the CMS ghost network regulation framework.
The 90-day verification rule and update timelines play a key role in audits. Delays in updates or missing documentation increase enforcement risk. Strong health plan provider data accuracy controls reduce audit exposure and help avoid penalties.
How Provider Directory Errors Affect Revenue Cycle Management
Directory errors directly disrupt claim processing and payment cycles. They create gaps in billing accuracy, compliance, and patient transparency.
Common Billing Issues Caused by Directory Errors
Provider directory errors under the No Surprises Act provider directory compliance lead to incorrect network status at the time of service. This results in claim denials, incorrect patient responsibility, and mismatched billing records. These issues often relate to CMS ghost network regulation issues.
Incorrect data also impacts eligibility checks and prior authorization. When provider details do not match payer records, claims are flagged or rejected. This creates delays and increases rework for billing teams.
Errors also affect coding and modifier usage. Billing staff may apply incorrect codes due to the wrong network or coverage details. This reduces claim accuracy and increases the risk of audit flags and resubmissions.
Financial and Operational Impact
Provider directory errors increase financial loss across the revenue cycle. Denials, delayed reimbursements, and write-offs reduce cash flow. This is directly linked to poor health plan provider data accuracy.
Operational burden also increases. Staff spend more time correcting claims, responding to payer requests, and fixing directory data. This slows down billing workflows and reduces productivity.
From a compliance view, errors may lead to civil monetary penalties (CMP) and inaccurate directory fines. Under the Consolidated Appropriations Act (CAA), enforcement is strict, and poor data management raises audit risk and financial exposure.
To manage the risk of inaccurate directory fines, practices should adopt Healthcare Audit Protection Services to maintain the documentation required for federal audit readiness.
Step-by-Step Workflow for Provider Directory Compliance
This section outlines a structured workflow for maintaining accurate provider directories. It supports the No Surprises Act provider directory compliance and reduces regulatory risk.
Data Collection and Validation
Start with accurate data collection from providers and internal systems. Capture demographics, specialties, locations, and network status. This step supports health plan provider data accuracy and reduces future discrepancies.
Validate data against credentialing records and payer systems. Cross-check information with contracts and enrollment details. This process ensures alignment with CMS ghost network regulation requirements.
Apply verification rules such as the 90-day verification rule. Confirm provider information at defined intervals. This reduces outdated entries and supports compliance with the Consolidated Appropriations Act (CAA).
Before submitting directory updates to payers, verify all provider information through your primary Physician Credentialing Services records to ensure absolute data accuracy.
Update Submission and Tracking
Submit updates immediately after any provider change. This includes location, contact details, or network participation. Timely updates support No Surprises Act provider directory compliance and reduce errors.
Track all submitted changes using audit logs or tracking systems. Maintain records of submission dates, changes made, and confirmation receipts. This helps demonstrate compliance during reviews.
Monitor update status across payer systems. Delays in updates can result in inaccurate directory fines and potential exposure to civil monetary penalties (CMP).
Ongoing Monitoring and Audit Preparation
Monitor provider directory data on a continuous basis. Regular checks help identify discrepancies early. This improves health plan provider data accuracy and reduces compliance risk.
Prepare for audits by maintaining complete documentation. Include verification logs, update records, and communication trails. This supports enforcement reviews under the CMS ghost network regulation.
Follow structured monitoring cycles aligned with the 90-day verification rule. Consistent oversight reduces the chance of violations under the No Surprises Act provider directory compliance and limits financial exposure from penalties.
Compliance Checklist to Avoid Federal Fines
This section outlines key actions to maintain No Surprises Act provider directory compliance. It helps reduce exposure to penalties, audits, and regulatory actions.
Provider Directory Compliance Checklist
Maintain accurate and updated provider records across all systems. This includes names, specialties, locations, and network status. Strong health plan provider data accuracy reduces claim errors and compliance risks.
Follow the 90-day verification rule for routine data validation. Update records within the required timeframe. Ensure alignment with the CMS ghost network regulation and internal credentialing systems.
Track all updates and maintain audit logs. Documentation must show when data was verified and changed. This supports defense against civil monetary penalties (CMP) and inaccurate directory fines.
Conduct periodic internal audits. Review directories for missing or outdated entries. Align processes with the Consolidated Appropriations Act (CAA) to reduce federal enforcement exposure.
Conclusion
Accurate provider directory data is now a core compliance requirement under the No Surprises Act provider directory compliance framework. Errors in directory data lead to claim denials, patient disputes, and exposure to civil monetary penalties (CMP) and regulatory audits.
Healthcare organizations must enforce the 90-day verification rule, timely updates, and strong data controls to maintain health plan provider data accuracy. Consistent monitoring and documented workflows reduce risk, protect revenue, and support long-term compliance.
FAQs
What is the No Surprises Act provider directory compliance?
It requires health plans and providers to maintain accurate, up-to-date directory data. This prevents incorrect billing and protects patients from unexpected out-of-network charges.
What is the 90-day verification rule?
Health plans must verify provider directory data at least every 90 days. This ensures accuracy and reduces outdated or incorrect provider listings.
What happens if provider directory data is inaccurate?
Inaccurate data can lead to claim denials, patient disputes, and billing errors. It may also result in audits, civil monetary penalties (CMP), and regulatory action.
What is a ghost network in healthcare?
A ghost network occurs when directories list providers who are unavailable or out-of-network. This creates access issues and violates CMS ghost network regulation standards.
How can providers maintain compliance with directory requirements?
They must update changes quickly, follow verification rules, and keep audit records. Strong coordination between billing, credentialing, and IT systems is essential.





