Have you ever wondered why a fully qualified physician or provider cannot see patients immediately, even after joining a practice? In 2026, more than half of hospitals and provider groups were expected to report revenue losses due to credentialing delays, with some practices losing $1,000 to $5,000 per clinician each day before seeing patients. Credentialing delays have a direct impact on claim approvals, billing efficiency, and patient access, causing administrative, coding, and billing teams to experience operational strain and frustration.
Proper provider credentialing ensures that healthcare practitioners are competent, licensed, and capable of providing safe care. It is required for in-network participation with insurance providers and protects practices from fraud, claim denials, and malpractice risk. Without effective credentialing, revenue cycle performance suffers, and patient care may be affected.
While the procedure can take 90–120 days on average and sometimes up to 180 days, understanding how long provider credentialing takes helps practices plan staffing, billing, and patient access while reducing financial losses. This blog will provide a clear definition of provider credentialing, its significance, and the differences between enrollment and credentialing, along with a high-level overview of the provider credentialing process. This will assist medical teams, administrators, and billing specialists in ensuring compliance and maximizing revenue.
What Is Provider Credentialing?
Provider credentialing is an effective process for ensuring that healthcare practitioners are qualified, licensed, and capable of giving safe care. This procedure is required for in-network participation with insurance carriers, compliance with federal and state standards, and protecting patients from unqualified physicians.
In 2026, over 55% of healthcare practices report delays in credentialing that directly affect revenue and patient access, with an average delay of 90–120 days. Understanding provider credentialing helps medical coders, billers, administrators, and clinicians reduce errors, prevent claim denials, and maintain operational efficiency.
How Do You Understand the Credentialing?
Credentialing is the verification of a healthcare provider’s qualifications, education, licenses, training, and professional history. It ensures providers meet healthcare credentialing requirements before they can deliver patient care in a facility or join insurance networks.
Key elements include:
- Education verification: medical school, residency, fellowships
- Licenses and board certifications state medical licenses and specialty boards.
- Employment and practice history, prior positions, hospital privileges
- Malpractice insurance coverage is current and verified.
- References and peer reviews professional recommendations.
Why Credentialing Is Mandatory
Credentialing is mandatory for several reasons:
1. Patient Safety: Only qualified and licensed providers are approved to deliver care.
2. Insurance Compliance: Providers must be credentialed to submit claims and receive reimbursement.
3. Legal Protection: Reduces risk of fraud, malpractice claims, and regulatory penalties.
4. Operational Efficiency: Proper credentialing prevents delays in claim processing and hospital privileges.
5. Reputation and Trust: Credentialed providers reinforce patient confidence and practice credibility.
Difference Between Credentialing and Enrollment
Understanding the distinction between credentialing and enrollment is critical for healthcare providers, billers, and administrators. Many practices face delays and claim denials because these two processes are often confused. In 2026, over 40% of credentialing-related claim denials occur due to incomplete enrollment documentation, highlighting the importance of knowing how each process functions.
Credentialing vs Enrollment
Credentialing verifies a healthcare provider’s qualifications, licenses, and training, ensuring they are authorized to practice safely. Enrollment registers the provider with insurance networks, allowing them to bill and receive reimbursement for patient services.
Credentialing is the verification of a provider’s qualifications and professional history. It ensures the provider is licensed, trained, and capable of delivering care safely. Key elements include:
- Verification of education, residency, and fellowship
- Licenses and board certifications
- Malpractice insurance coverage
- Hospital privileges and work history
Enrollment, in contrast, is the process of registering the provider with insurance networks. Enrollment allows the provider to bill for services rendered to insured patients. Key steps include:
1. Submission of the insurance application with practice details
2. Verification of documents, including licenses and liability coverage
3. Approval and assignment of provider identification numbers
Key Differences:
Focus: Credentialing verifies qualifications; enrollment allows reimbursement.
Outcome: Credentialed providers can practice; enrolled providers can bill insurance.
Timeline: Credentialing can take 90–120 days; enrollment may take 30–60 days after credentialing.
Stakeholders: Credentialing involves healthcare facilities and credentialing bodies; enrollment involves providers and insurance payers.
Who Needs Credentialing
Provider credentialing ensures all relevant healthcare personnel meet the required standards to deliver safe, compliant, and reimbursable care. This process applies to multiple categories of healthcare staff and facilities. Providers who plan to treat patients within hospitals must also complete the hospital privileging process, which determines the clinical services they are authorized to perform.
Healthcare Providers
Physicians, nurse practitioners, physician assistants, therapists, and specialists must complete provider credentialing to practice safely and bill insurance companies. Proper credentialing verifies education, licenses, certifications, and work history.
Facilities and Organizations
Hospitals, clinics, surgery centers, and outpatient facilities must ensure their providers are credentialed. Facilities rely on credentialing to meet payer requirements, reduce liability, and maintain accreditation.
Ancillary Staff
Pharmacists, lab technicians, imaging staff, and other support personnel require credentialing for specific roles. This ensures compliance with healthcare credentialing requirements and supports accurate billing and patient safety.
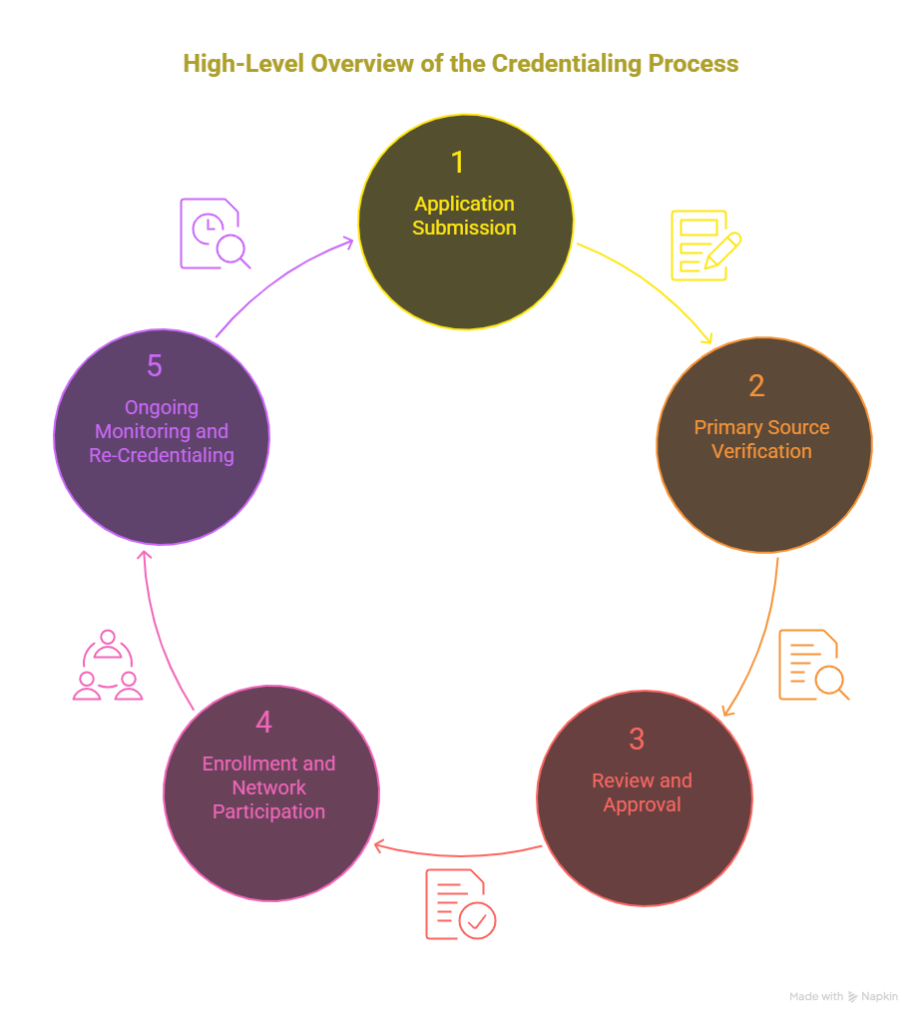
High-Level Overview of the Credentialing Process
The provider credentialing process involves multiple structured steps to verify and approve healthcare providers while ensuring compliance with payer and regulatory standards.
Step 1: Application Submission
Providers submit detailed credentialing applications through platforms such as the CAQH credentialing system, including education, licenses, certifications, employment history, and malpractice insurance. Accuracy at this stage reduces delays and rejections.
Step 2: Primary Source Verification
Healthcare organizations contact medical schools, licensing boards, previous employers, and professional references. Verification confirms the authenticity of submitted credentials and work history.
Step 3: Review and Approval
Credentialing committees review verified data against organizational standards. Approved providers gain authorization to practice and begin facility-specific operations.
Step 4: Enrollment and Network Participation
Providers apply to join insurance networks to receive reimbursement. Enrollment ensures access to patient populations and compliance with payer requirements.
Step 5: Ongoing Monitoring and Re-Credentialing
Credentialing is continuous. Providers must update licenses, certifications, and privileges. Periodic medical re-credentialing ensures providers continue meeting healthcare credentialing requirements and payer compliance standards.
Risks of Improper Credentialing
Improper provider credentialing often results from documentation gaps and common credentialing mistakes that delay provider approval, creating risks for patient care and financial operations. Understanding these risks helps healthcare teams prioritize accurate and timely credentialing.
Patient Safety Risks
Inaccurate credentialing may allow unqualified providers to deliver care. This increases the likelihood of medical errors, misdiagnosis, and adverse patient outcomes. According to 2026 healthcare reports, 12–15% of preventable medical errors involve lapses in provider verification.
Financial and Legal Risks
Healthcare organizations can face claim denials, delayed reimbursements, and fines from insurers if credentialing is incomplete. Legal exposure rises when malpractice claims involve providers who were not properly credentialed.
Organizational Reputation Risks
Hospitals and clinics may lose credibility with patients and payers when credentialing standards are weak. Negative publicity or regulatory sanctions can reduce patient trust and limit network participation.
Final Thought
Provider credentialing is essential for ensuring that healthcare practitioners are qualified, licensed, and capable of delivering safe patient care. Accurate credentialing supports compliance, reduces claim denials, and protects both patients and healthcare organizations from financial and legal risk.
By implementing structured credentialing processes and ongoing monitoring, healthcare facilities can maintain operational efficiency, safeguard their reputation, and ensure access to qualified providers. To maintain compliance and accelerate the revenue cycle, many healthcare groups rely on professional Physician Credentialing Services to manage the technical complexities of payer enrollment.
FAQs
What is provider credentialing?
Provider credentialing is the process of verifying a healthcare provider’s qualifications, licenses, and training to ensure safe and compliant patient care.
Why is credentialing mandatory for healthcare providers?
Credentialing is required to maintain patient safety, meet insurance compliance, reduce legal risk, and ensure accurate billing and reimbursement.
How long does the provider credentialing process take?
The process typically takes 90–120 days, with some cases extending up to 180 days, depending on verification and approval timelines.
Who needs provider credentialing?
Physicians, specialists, nurse practitioners, therapists, hospitals, clinics, and ancillary staff must be credentialed to practice safely and bill insurers.
What are the risks of improper credentialing?
Incomplete credentialing can lead to patient safety issues, claim denials, financial losses, legal exposure, and damage to organizational reputation.





